Cryptosporidiosis, often referred to as “Crypto,” is a parasitic infection that primarily affects the gastrointestinal tract and causes watery diarrhea. It is caused by the microscopic parasite Cryptosporidium parvum, which belongs to the Phylum Apicomplexa, Order Eimeriida, and Genus Cryptosporidium. This infection spreads mainly through the ingestion of contaminated water or food containing sporulated oocysts, making it a significant public health concern worldwide.
What is Cryptosporidiosis?
Cryptosporidiosis is an intestinal disease caused by Cryptosporidium parvum. The parasite exists as a sporulated oocyst that is colorless, transparent, and either oval or spherical in shape. Each oocyst contains four crescent-shaped sporozoites, which are the infective form that invades host cells. Once ingested, the parasite resides primarily in the small intestine, within the epithelial tissue of the microvillus region.
Although the disease can affect anyone, people with weakened immune systems—such as those with HIV/AIDS, transplant patients, or individuals on immunosuppressive drugs—are at higher risk for severe and chronic infections.
Habitat and Geographical Distribution
Cryptosporidium parvum is an intracellular parasite, found inside the epithelial cells of the small intestine. Cryptosporidiosis is found worldwide, with outbreaks reported in both developed and developing countries. Transmission is particularly common in areas with contaminated drinking water, poor sanitation, or recreational water exposure such as swimming pools.
Life Cycle of Cryptosporidium parvum
The life cycle of C. parvum is complex and includes both asexual and sexual stages:
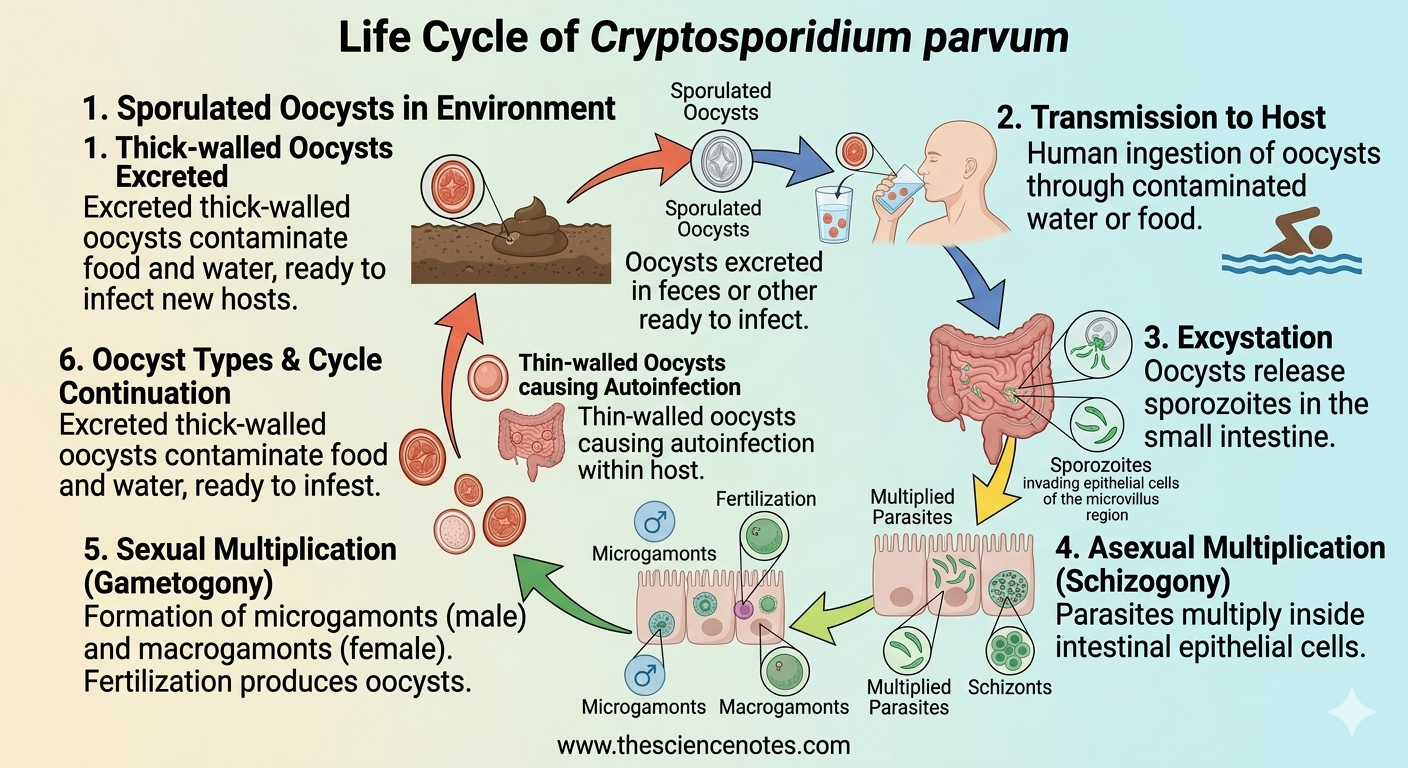
Oocyst Excretion: Sporulated oocysts containing four sporozoites are shed in feces and may also appear in respiratory secretions.
Transmission: Humans ingest oocysts through contaminated water or food.
Excystation: In the host, sporozoites are released from the oocyst and invade epithelial cells of the small intestine or, in some cases, the respiratory tract.
Asexual Multiplication (Schizogony): Parasites multiply inside host cells, producing merozoites.
Sexual Multiplication (Gametogony): Merozoites differentiate into male (microgamonts) and female (macrogamonts) forms. Fertilization produces oocysts.
Oocyst Types:
Thick-walled oocysts: Commonly excreted in feces, capable of surviving outside the host.
Thin-walled oocysts: Involved in autoinfection within the host, allowing the infection to persist.
Cycle Continuation: Excreted oocysts contaminate the environment, leading to new infections when ingested by a susceptible host.
The infective oocysts are resistant to many common disinfectants, which is why waterborne outbreaks are frequent.
Clinical Manifestations of Cryptosporidiosis
Symptoms typically appear 2–10 days after exposure (average incubation: 7 days). The most common symptom is watery diarrhea, which may be accompanied by:
Stomach cramps or abdominal pain
Dehydration
Nausea and vomiting
Fever
Weight loss
Some infected individuals, especially those with strong immune systems, may be asymptomatic. In healthy individuals, symptoms generally last 1–2 weeks, whereas immunocompromised patients may develop chronic, severe, or potentially fatal infections.
High-risk groups include:
People with HIV/AIDS
Patients with inherited immune deficiencies
Cancer or transplant patients on immunosuppressive drugs
While the small intestine is the primary site of infection, in vulnerable individuals, Cryptosporidium can affect other parts of the gastrointestinal or respiratory tracts.
Laboratory Diagnosis
Several methods can confirm cryptosporidiosis:
Microscopy:
Examine at least three stool samples for oocysts.
Concentration techniques like formalin-ethyl acetate sedimentation improve visibility.
Wet mounts with iodine or acid-fast staining show oocysts stained red with safranin.
Enzyme Immunoassays (EIA): Detect cryptosporidial antigens.
Immunofluorescence Microscopy: Sensitive detection of oocysts in stool or other samples.
PCR: Molecular confirmation for precise identification, especially in outbreaks.
Treatment of Cryptosporidiosis
Most healthy individuals recover without treatment, and diarrhea can be managed by:
Maintaining hydration: Drink plenty of fluids, including oral rehydration solutions.
Anti-diarrheal medication: Only under guidance of a healthcare provider.
Nitazoxanide: Can reduce severity and duration of diarrhea.
For immunocompromised patients, treatment may require supportive care, antiretroviral therapy (for HIV), and other interventions to manage chronic infection.
Prevention and Control
Preventing cryptosporidiosis relies on good hygiene and safe water practices:
Water Safety: Boiling water or using chlorine disinfection effectively kills Cryptosporidium. Ultraviolet (UV) light at low doses also inactivates oocysts.
Food Safety: Wash hands, fruits, and vegetables to prevent ingestion of oocysts.
Personal Hygiene: Avoid swallowing water in swimming pools or recreational water. Infected individuals should not swim until at least two weeks after diarrhea stops.
Environmental Control: Proper sewage disposal and avoiding contamination of drinking water sources.
By following these measures, both sporadic cases and large-scale outbreaks of cryptosporidiosis can be minimized.
Key Takeaways
Cryptosporidiosis is caused by Cryptosporidium parvum, a microscopic parasite that infects the small intestine.
Infection spreads primarily through contaminated water and food containing sporulated oocysts.
Symptoms include watery diarrhea, dehydration, abdominal pain, and fever, with severity depending on immune status.
Diagnosis involves microscopy, EIA, immunofluorescence, or PCR.
Healthy individuals often recover without medication, but Nitazoxanide may be used in symptomatic cases.
Prevention relies on water disinfection, food hygiene, and avoiding exposure to contaminated water.
Understanding the life cycle and transmission of Cryptosporidium parvum is essential for effective public health measures, especially in areas with contaminated water supplies and immunocompromised populations.