Syphilis: The Silent Resurgence of a Curable Infection
Syphilis is often viewed as a disease of the distant past. However, recent data from the United States and globally indicates a alarming trend: syphilis infection rates have been steadily increasing over the past two decades. In 2020 alone, 41,655 new cases were reported in the US.
The most crucial fact about syphilis is that it is curable, yet its symptoms are notorious for mimicking other common ailments or vanishing entirely, leading to many undiagnosed cases. Understanding how the infection spreads, recognizing its progressive stages, and knowing when to get tested are essential steps in halting this resurgence and protecting your long-term health.
What is Syphilis?
Syphilis is a complex infection caused by the bacterium Treponema pallidum. It belongs to the class of sexually transmitted infections (STIs) and is primarily acquired through genital, oral, or anal sex.
The infection can be transmitted when someone has direct contact with an active syphilis sore (chancre) on another person. Crucially, transmission can occur even if a person doesn’t have an active sore, especially during the secondary and latent stages of infection.
While transmission is most common among adults, it is also highly dangerous for pregnant individuals. If left untreated, syphilis can pass from a pregnant person to their fetus, a condition known as Congenital Syphilis.
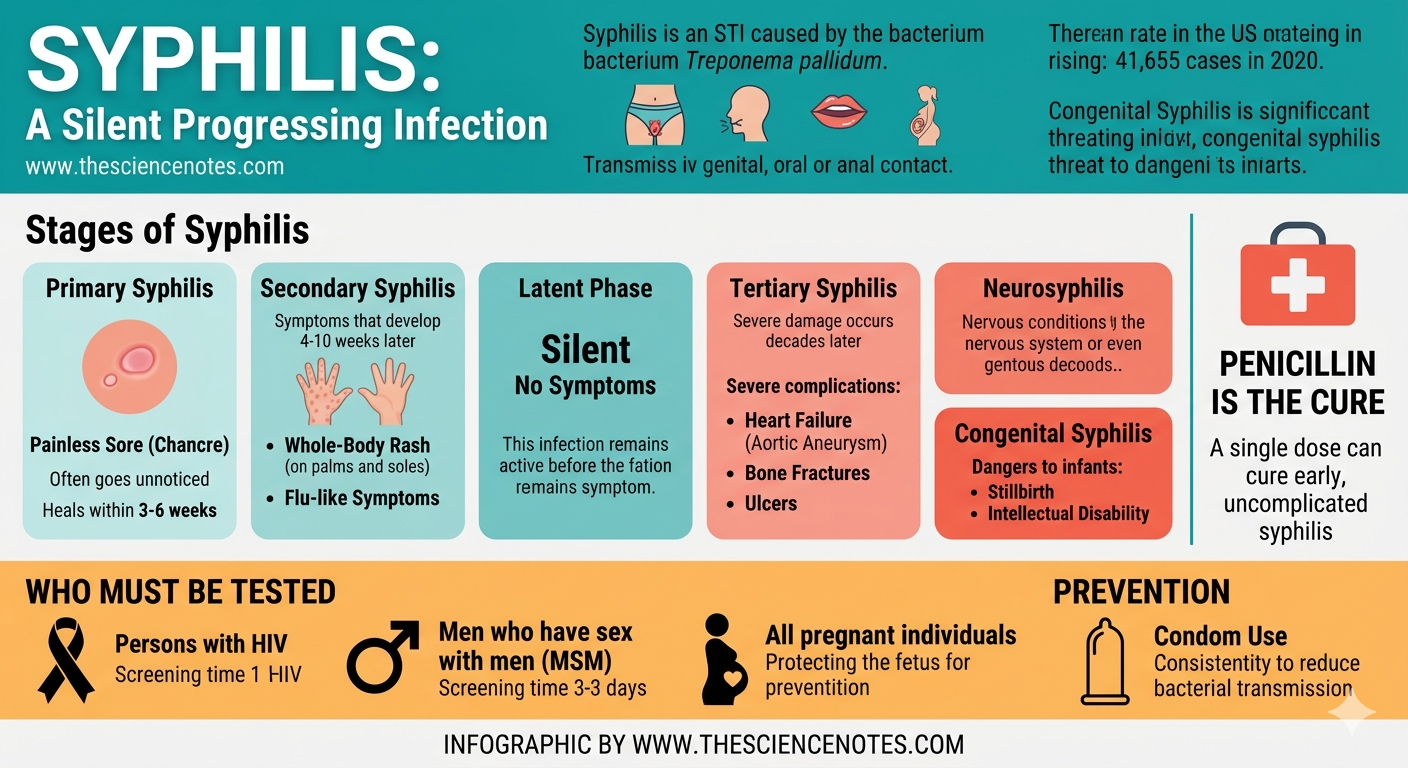
The Progressions of Syphilis: From Minor Sore to Severe Complications
Syphilis is known for its ability to progress through multiple, distinct stages if not treated early. These stages vary significantly in symptoms, severity, and the potential for long-term damage.
1. Primary Syphilis (The Entry Point)
The first sign of syphilis is usually a single sore called a chancre.
Appearance: This chancre is typically firm, round, and painless. It appears where the bacteria entered the body—usually on the genitals, anus, mouth, or throat.
The Hidden Danger: Chancres can occur deep in the rectum or on the cervix, making them easy to miss. Even if noticed, they often heal completely on their own in 3 to 6 weeks. Because they don’t hurt, many people skip treatment, believing the problem has resolved itself. However, this means the infection has simply moved to the next stage.
2. Secondary Syphilis (The Systemic Spread)
Without treatment during the primary stage, about 25% of patients develop secondary syphilis. This stage indicates the T. pallidum bacteria has spread into the bloodstream. Symptoms typically begin 4 to 10 weeks after the primary chancre has healed.
The “Whole-Body” Symptoms:
A skin rash that may appear on the torso, palms of the hands, or soles of the feet. This rash usually doesn’t itch.
Flu-like symptoms, including fever, swollen lymph glands, sore throat, and headaches.
Muscle aches and fatigue.
Patches of hair loss.
3. Latent Syphilis (The Dormant Phase)
After the secondary stage symptoms subside, the infection enters a latent period. During this phase, there are no visible signs or symptoms whatsoever.
The Deception: The infection is still present and active in the body, slowly causing damage to internal organs, including the brain, heart, and nerves. This period can last for years, or even decades.
4. Tertiary Syphilis (The Damage Phase)
Tertiary syphilis occurs in a small percentage of untreated patients, appearing years or decades after the initial infection. This stage represents a multi-organ disaster:
Cardiovascular Issues: Syphilis can cause an aneurysm (enlargement) of the aorta, leading to heart failure and severe heart disease.
Gummas: Development of painful skin ulcers and destruction of bones.
When the System is Affected: Neurosyphilis and Congenital Syphilis
Two specific complications of syphilis demand an immediate, specialized response:
Neurosyphilis: An infection of the central nervous system that can occur at any stage of a syphilis infection. Symptoms can include meningitis, stroke, sudden hearing loss or blindness, paralysis, and dementia. This requires intensive medical intervention.
Congenital Syphilis: A mother passes syphilis to her baby during pregnancy. This is a severe, life-threatening condition. Congenital syphilis can cause stillbirth or infant death. Surviving children often suffer from:
Teeth, bone, and facial abnormalities.
Visual impairment or blindness.
Deafness.
Severe intellectual disability.
Diagnosis, Treatment, and Cure: The Penicillin Solution
How is Syphilis Diagnosed?
Because its progressive stages have such varied symptoms, laboratory confirmation is necessary. Doctors use blood tests that look for specific antibodies your immune system produces to fight the T. pallidum bacteria. Common tests include the RPR (Rapid Plasma Reagin) or VDRL (Venereal Disease Research Laboratory) test. Some highly specialized labs can use PCR testing to identify the bacterial DNA directly.
The Treatment of Choice
The solution to a syphilis infection is surprisingly straightforward: Antibiotics.
Penicillin is the cure. It is typically given as an intramuscular injection (or intravenously for complex cases).
Single-Dose Cure: A single dose of penicillin is often curative for early, uncomplicated cases.
Alternatives: Patients with a documented penicillin allergy can be given alternative antibiotics or undergo a desensitization procedure so they can safely receive penicillin.
Prevention and Who Should Be Tested
How to Prevent Syphilis
The most effective way to prevent syphilis and other STIs is to consistently and correctly use condoms during genital, oral, and anal sex. Condoms provide a barrier, reducing direct contact with an active chancre.
Who Must Be Tested?
Because the early symptoms (the painless chancre) can be easily missed, active screening is crucial. Syphilis testing is recommended for:
Anyone with Symptoms: If you notice a sore on your genitals or have a whole-body rash, seek testing immediately.
Sexual Partners: If you are diagnosed with syphilis, all recent sexual partners must be notified and tested.
High-Risk Groups: Individuals with HIV or men who have sex with men (who represent about half of all new cases in the US) should be screened at least once a year, even if they have no symptoms.
All Pregnant Individuals: Universal screening is required during the first prenatal visit. Those in high-prevalence areas should be re-tested at 28 weeks of gestation. Early detection during pregnancy is the only way to prevent congenital syphilis and protect the baby.
Conclusion
Syphilis is a silent resurgent threat, but it is one we know how to stop. It progresses from a painless entry to catastrophic systemic damage only if we allow it to go untreated. By consistently using protection, recognizing the early symptoms that so often go unnoticed, and committing to proactive testing—especially for at-risk groups and pregnant mothers—we can secure a cure and halt the transmission of this entirely preventable disease.
References:
Data on case numbers and populations adapted from CDC and provided sources.