Type 1 diabetes is a chronic condition that requires lifelong management and a deep understanding of how the body processes energy. While many people confuse it with Type 2 diabetes, the two conditions have vastly different origins. Specifically, Type 1 diabetes is an autoimmune disease where the body’s immune system mistakenly attacks itself. Because of this, the pancreas loses its ability to produce insulin, leading to dangerously high blood glucose levels.
Currently, Type 1 diabetes accounts for approximately 5% to 10% of all diabetes cases. Globally, it affects about 8.4 million people, including 2 million individuals in the United States alone. Although it is most commonly diagnosed in children and adolescents, it is important to remember that this condition can develop at any age.
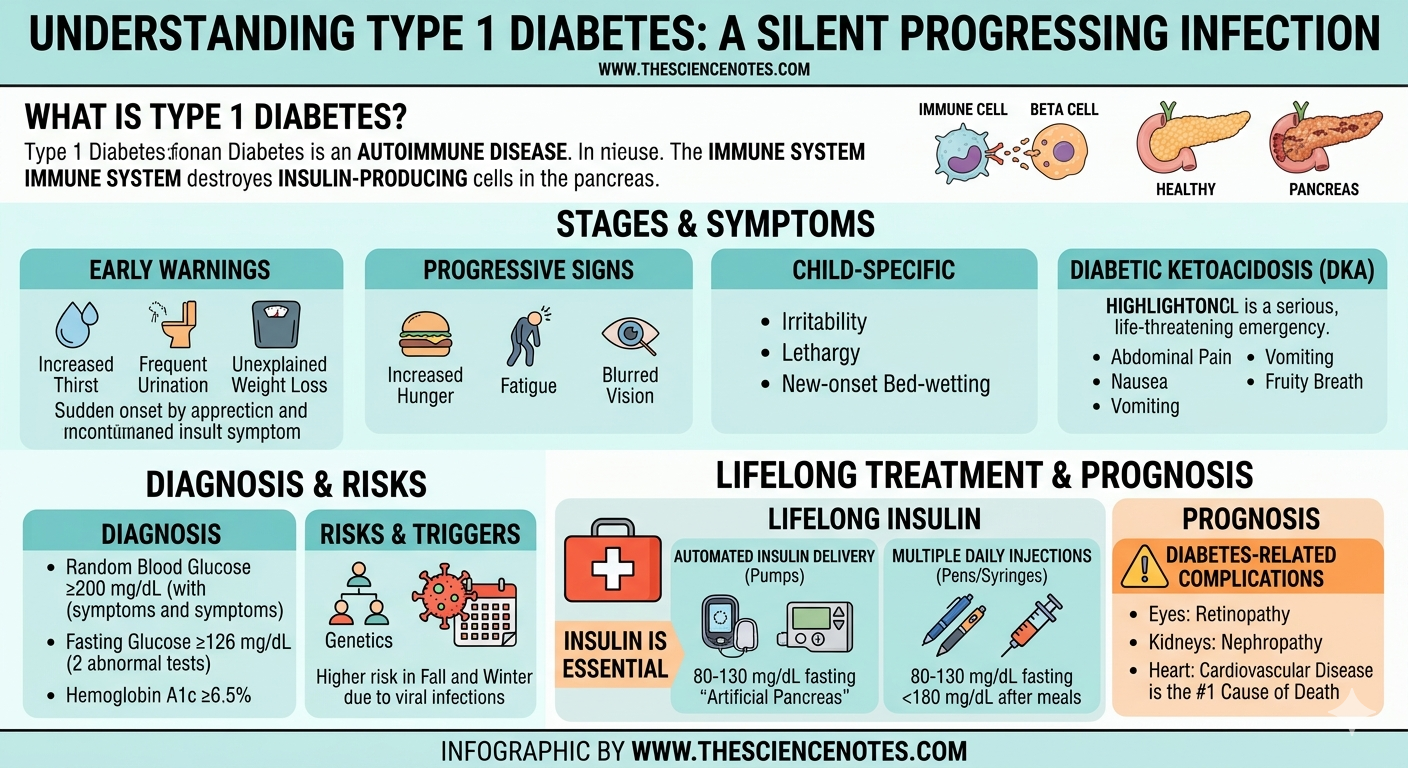
What is Type 1 Diabetes?
At its core, Type 1 diabetes occurs when the immune system destroys insulin-producing cells (beta cells) in the pancreas. Insulin is a vital hormone that acts as a bridge, allowing sugar from the food we eat to enter our cells for energy.
Without insulin, glucose remains trapped in the bloodstream. Consequently, the body begins to starve at a cellular level, even if the person is eating plenty of food. If left untreated, this buildup of sugar can cause severe damage to the heart, kidneys, eyes, and nerves.
Common Risk Factors for Type 1 Diabetes
Many patients wonder why they developed this condition. While research is ongoing, we know that genetics and environment play the largest roles.
1. Genetic Predisposition
If you have a first-degree relative—such as a parent or sibling—with the disease, you are more likely to develop it yourself. However, statistics show that 85% of people with Type 1 diabetes actually have no family history of the condition. This suggests that while genes provide the “blueprint,” something else must trigger the disease.
2. Environmental Triggers
Interestingly, Type 1 diabetes is more frequently diagnosed during the fall and winter months. Many experts believe that viral infections, which are more prevalent in cold weather, may act as a trigger. These infections can cause the immune system to malfunction and begin attacking the pancreas.
Recognizing the Symptoms of Type 1 Diabetes
The symptoms of Type 1 diabetes often appear suddenly. If you notice these signs, you should consult a healthcare provider immediately.
Extreme Thirst and Frequent Urination: As the kidneys try to flush out excess sugar, you may feel dehydrated and need to use the bathroom constantly.
Unexplained Weight Loss: Because the body cannot use glucose for energy, it begins burning fat and muscle instead.
Increased Hunger and Fatigue: Even after eating, you may feel tired because your cells aren’t getting the energy they need.
Blurred Vision: High blood sugar levels can pull fluid from the lenses of your eyes, affecting your ability to focus.
Warning Signs in Children
In young children, parents should look for increased irritability, lethargy, or a sudden onset of bed-wetting in a child who was previously potty-trained.
The Danger of Diabetic Ketoacidosis (DKA)
A significant number of patients—up to 44% of children and 23% of adults—are only diagnosed after they develop Diabetic Ketoacidosis (DKA). This is a life-threatening medical emergency.
When the body cannot use sugar, it breaks down fat too quickly, producing acidic chemicals called ketones. Symptoms of DKA include:
Severe abdominal pain.
Nausea and vomiting.
Fruity-smelling breath.
Confusion or rapid breathing.
DKA requires immediate hospitalization and treatment with intravenous insulin to stabilize blood sugar and pH levels.
How Doctors Diagnose Type 1 Diabetes
To confirm a diagnosis, doctors look for specific markers in the blood. If you show symptoms, a random blood glucose level of 200 mg/dL or higher is a primary indicator. For those without obvious symptoms, diagnosis requires two abnormal results from the following tests:
Fasting Blood Glucose: 126 mg/dL or higher.
A1c Test: A hemoglobin A1c of 6.5% or higher, which measures average blood sugar over three months.
Antibody Testing: Because Type 1 is an autoimmune disease, 90% to 95% of patients will have specific antibodies in their blood that target the pancreas.
Modern Treatment and Insulin Management
Because the pancreas no longer functions, people with Type 1 diabetes need lifelong insulin treatment. Fortunately, medical technology has made management much more precise.
Automated Insulin Pumps
Most patients in the U.S. now use an automated insulin pump combined with a continuous glucose monitor (CGM). The CGM is a sensor attached to the skin that records glucose levels every few minutes. The pump then automatically adjusts the insulin dose to keep levels within the target range.
Fasting Target: 80 to 130 mg/dL.
Post-Meal Target: Less than 180 mg/dL.
Multiple Daily Injections (MDI)
Alternatively, some patients use an insulin pen or syringe. This method involves taking long-acting insulin once a day and rapid-acting insulin at every meal. Regardless of the method, working with a registered dietitian is essential to develop an individualized eating plan and master carbohydrate counting.
Long-Term Prognosis and Complications
Living with Type 1 diabetes is a lifelong journey. Unfortunately, more than 95% of patients develop at least one diabetes-related complication over time. These issues typically involve:
The Heart: Cardiovascular disease is the leading cause of death for those with Type 1.
The Kidneys and Eyes: Chronic high sugar can lead to kidney failure or blindness.
Peripheral Nerves: Damage to the nerves, especially in the feet, can cause numbness or pain.
While the life expectancy for those with the condition is currently 8 to 10 years shorter than those without it, the outlook is improving. By maintaining blood glucose levels within the target range, you can significantly reduce the risk of these complications.
For more information : https://diabetes.org/