Introduction
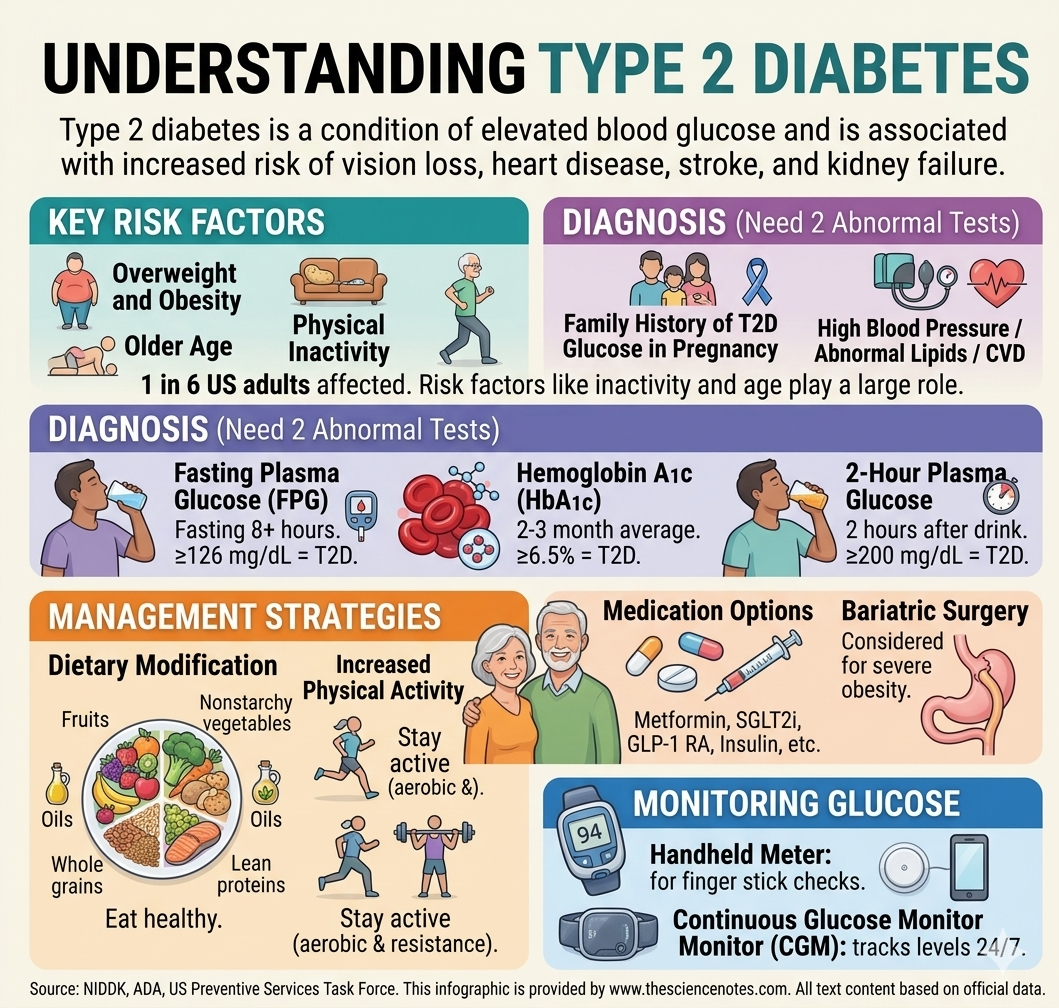
Type 2 diabetes is no longer just a “lifestyle disease”—it is a global health crisis. Characterized by elevated blood glucose (sugar) levels, this chronic condition affects approximately 14% of the population worldwide and nearly 1 in 6 adults in the United States.
If left unmanaged, the consequences are severe, ranging from irreversible vision loss and nerve damage to life-threatening events like heart disease, stroke, and kidney failure. However, with modern diagnostic tools and a proactive approach to treatment, living a long, healthy life is entirely possible. This guide covers everything you need to know about navigating a type 2 diabetes diagnosis.
What is Type 2 Diabetes?
At its core, type 2 diabetes is a disorder of how the body uses energy. In a healthy body, the pancreas produces insulin, a hormone that acts like a key to let blood sugar into your cells for use as energy.
In type 2 diabetes, the body either doesn’t produce enough insulin or the cells stop responding to it properly (known as insulin resistance). When the “key” no longer works, sugar builds up in the bloodstream instead of fueling the cells. Over time, this high glucose causes systemic inflammation and damage to blood vessels throughout the body.
Common Risk Factors for Type 2 Diabetes
While genetics play a significant role, several factors increase the likelihood of developing the condition. Understanding these can help you take preventative action:
Overweight and Obesity: This is the leading risk factor. Excess body fat, particularly around the abdomen, is linked to insulin resistance.
Physical Inactivity: Leading a sedentary lifestyle contributes significantly to the development of type 2 diabetes. Movement helps your body use glucose directly.
Older Age: The risk increases as you get older, particularly after age 35, partly due to the body’s natural decreased ability to process glucose.
Family History: Having a parent or sibling with type 2 diabetes drastically increases your risk.
Gestational Diabetes: A history of having high blood glucose levels during pregnancy makes a woman and her child more susceptible to type 2 diabetes later in life.
Associated Health Conditions: Conditions such as high blood pressure (hypertension), abnormal blood lipid (fat/cholesterol) levels, and existing cardiovascular disease are strong indicators of elevated diabetes risk.
Symptoms and Warning Signs
One of the most dangerous aspects of type 2 diabetes is its “silent” nature. Most patients have no symptoms when they are first diagnosed. The body often adapts to rising sugar levels so slowly that the changes go unnoticed for years. By the time symptoms appear, damage may already be occurring.
When symptoms do present, they may include:
Polyuria (Frequent Urination): High blood sugar pulls fluid from your tissues, leading to excessive fluid loss.
Polydipsia (Extreme Thirst): As your body uses water to flush out excess sugar, you become chronically dehydrated.
Fatigue: Feeling lethargic because cells aren’t getting the glucose they need for energy.
Blurry Vision: High sugar levels can cause the lenses of your eyes to swell, distorting your focus.
Unintentional Weight Loss: When the body can’t use glucose for fuel, it begins to break down muscle and fat for energy, causing you to lose weight.
How Type 2 Diabetes is Diagnosed
Because symptoms can be elusive, clinical testing is the only definitive way to identify the condition. A diagnosis typically requires two abnormal results from the following tests, performed on separate days:
1. Fasting Plasma Glucose (FPG)
This test measures your blood sugar after you have refrained from eating or drinking (except water) for at least 8 hours. This is often the first test given for screening.
Result: A blood glucose level of 126 mg/dL or higher indicates type 2 diabetes.
2. Hemoglobin A1c (HbA1c)
Often simply called “A1c,” this is a crucial metric. It provides an average of your blood glucose levels over the past 2 to 3 months by measuring the percentage of blood sugar that is “stuck” to hemoglobin in your red blood cells. It does not require fasting.
Result: An HbA1c of 6.5% or higher indicates type 2 diabetes.
3. Two-Hour Plasma Glucose (Oral Glucose Tolerance Test – OGTT)
During an OGTT, your blood is tested after 8 hours of fasting and again 2 hours after you drink a specific high-sugar solution. It is the most sensitive test for prediabetes and diabetes.
Result: A blood glucose level of 200 mg/dL or higher indicates type 2 diabetes.
Recommended Lifestyle Modifications for Type 2 Diabetes
Lifestyle changes are the absolute cornerstone of diabetes management. For many people, these changes are powerful enough to keep blood sugar within target ranges, sometimes without needing heavy medication.
Dietary Modification: The Foundation of Control
A “diabetes diet” is not a temporary fix; it is a permanent lifestyle of mindful, nutritional excellence. Key goals are reducing carbohydrate surges and promoting fiber intake. Focus on:
Fiber-rich Carbohydrates: Skip white bread and sugary cereals for whole grains like quinoa, oats, and brown rice. Legumes (beans and lentils) and fruits are also excellent sources.
Nonstarchy Vegetables: Load your plate with leafy greens, broccoli, peppers, mushrooms, and zucchini.
Lean Proteins: Prioritize fish (rich in omega-3s), poultry, and plant-based proteins over red meat.
Healthy Fats: Replace saturated fats with unsaturated versions found in olive oil, avocados, nuts, and seeds.
Increased Physical Activity: Activating Muscle Glucose Uptake
Exercise makes your cells more sensitive to insulin, meaning your body needs less insulin to process the same amount of glucose. Aim for:
Aerobic Exercise: Activities like brisk walking, swimming, or cycling for at least 150 minutes per week (e.g., 30 minutes, 5 days a week).
Resistance Training: Weight lifting or bodyweight exercises (like squats and pushups) twice a week help build muscle tissue, which is one of the biggest consumers of glucose in the body.
How Is Type 2 Diabetes Treated and Monitored?
When lifestyle changes alone are not sufficient to reach target HbA1c levels, healthcare providers will turn to pharmacological interventions.
Medical Treatment and Innovations
First-Line Medications:
Metformin: This is almost always the first medication prescribed. It lowers blood sugar by reducing the amount of glucose the liver releases and improving insulin sensitivity.
SGLT2 Inhibitors: If a patient also has cardiovascular disease, high blood pressure, or kidney disease, sodium-glucose cotransporter 2 (SGLT2) inhibitors may be prescribed early. These medications work by preventing the kidneys from reabsorbing glucose, allowing excess sugar to be flushed out through urination.
GLP-1 Receptor Agonists (GLP-1 RAs): Another powerful tool, especially beneficial for heart and kidney health and potent weight loss. These mimic a hormone that stimulates insulin release, suppresses glucagon (which raises sugar), and slows digestion.
Additional Medications: If more control is needed, other options include:
Dual GIP/GLP-1 RAs: A novel class of drug that combines two hormones to improve insulin production and fullness even further.
Dipeptidyl Peptidase 4 (DPP-4) Inhibitors.
Sulfonylureas: These stimulate the pancreas to make more insulin (though they carry a higher risk of hypoglycemia, or low blood sugar).
Thiazolidinediones.
Insulin Treatment: About one-third of all patients with type 2 diabetes will require insulin therapy at some point in their life. Insulin is necessary when the body stops making enough of its own to maintain normal levels. It can be delivered through injections, pens, or an insulin pump.
Bariatric Surgery: Weight loss surgery can be a game-changer for people with both obesity and type 2 diabetes. It promotes extreme weight loss, which often改善 (improves) metabolic health, and in some cases, can even lead to diabetes remission.
Monitoring Blood Glucose Levels
Self-monitoring is the only way to know if your treatment plan is working from day to day. There are two primary methods:
Handheld Glucometer (BGM): This method involves using a lancet to get a small blood sample (finger stick) which is placed on a test strip in a handheld meter. It provides a “snapshot” of your blood sugar at that exact moment.
Continuous Glucose Monitor (CGM): This advanced system uses a tiny sensor placed under the skin (usually on the arm or abdomen) that continuously tracks glucose levels. It transmits results in real-time to a smartphone or receiver, providing 24/7 visibility into glucose trends and sending alerts if levels become dangerously high or low.
Screening and Prevention: Who Should Be Tested?
Early detection is the key to preventing the devastating complications of diabetes. If you know you have prediabetes, you have a vital window of opportunity to reverse course. Guidelines vary slightly between major health organizations:
US Preventive Services Task Force (USPSTF): Recommends screening for adults aged 35 to 70 who have overweight (BMI ≥25) or obesity (BMI ≥30). If results are normal, repeat screening every 3 years.
American Diabetes Association (ADA): Recommends screening for all adults aged 35 years or older at least every 3 years. Testing should be done annually or every 1–3 years for adults with gestational diabetes history or with overweight/obesity plus additional risk factors (like a first-degree family member with type 2).
The Importance of Screening in Prediabetes
An annual screening is mandatory for individuals with prediabetes (defined as higher-than-normal blood glucose levels that do not yet meet the criteria for type 2). Prediabetes can be managed with lifestyle modifications, which can prevent or delay the progression to full-blown type 2 diabetes.
For More Information
Managing a chronic condition like type 2 diabetes can be overwhelming, but you are not alone. Resources are available through healthcare providers, diabetes support groups, and authoritative organizations.
Learn more at: National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
Disclaimer: This information is for educational purposes only and does not replace medical advice from a professional healthcare provider.