Varicoceles are a common yet often misunderstood medical condition that affects millions of men in the United States. While the term may sound complex, the condition is essentially a circulatory issue within the male reproductive system. Understanding how varicoceles develop, their impact on fertility, and the available treatment options is crucial for long-term reproductive health.
What is a Varicocele?
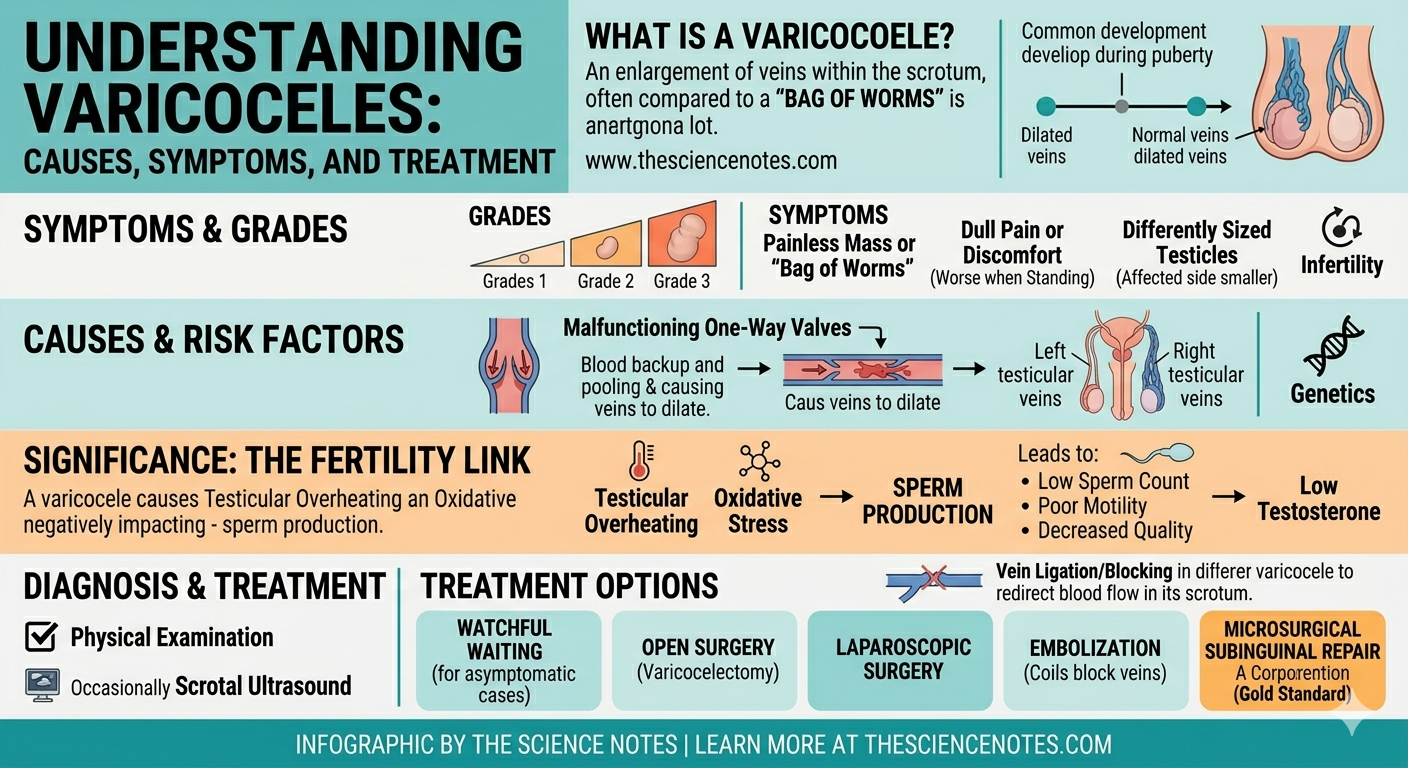
A varicocele is an enlargement of the veins within the scrotum—the loose bag of skin that holds the testicles. Specifically, it involves the pampiniform plexus, a network of small veins that transport oxygen-depleted blood away from the testicle.
Think of a varicocele as being similar to a varicose vein you might see in a leg. These enlargements are remarkably common, present in approximately 20% of men. They typically appear during puberty and may grow larger or more noticeable as a man ages.
The Three Grades of Varicoceles
Medical professionals classify varicoceles into three “grades” based on their size and visibility:
Grade 1: The smallest form; these are not visible and can only be detected by a doctor during a physical exam, often while the patient performs a breathing maneuver (Valsalva maneuver).
Grade 2: Medium-sized; these are still not visible but can be easily felt by a healthcare professional without special maneuvers.
Grade 3: The largest form; these can be seen through the skin and are often described as feeling like a “bag of worms” next to the testicle.
Symptoms and Warning Signs
In many cases, a varicocele is “silent,” producing no obvious symptoms. However, when symptoms do occur, they typically include:
Scrotal Pain: Often described as a dull, aching discomfort. This pain usually worsens when standing or after physical exertion late in the day, but it is typically relieved by lying down.
Visible or Palpable Mass: A Grade 3 varicocele may look like twisted veins or feel like a soft mass above the testicle.
Testicular Atrophy: You may notice that the affected testicle (usually the left side) is significantly smaller than the other.
Fertility Issues: For some men, the first sign of a varicocele is difficulty fathering a child.
When to See a Doctor
If you notice any swelling, a lump in your scrotum, or a difference in the size of your testicles, it is important to schedule an appointment with a urologist. While varicoceles are usually harmless, a professional diagnosis is required to rule out more serious conditions like infections or trauma.
Causes and Risk Factors
The exact cause of varicoceles remains somewhat of a medical mystery, but the mechanics of the condition are well-understood.
The Role of Vein Valves
The testicular arteries deliver oxygen-rich blood to the testicles, while the veins carry oxygen-depleted blood back to the heart. To prevent blood from flowing backward, these veins contain one-way valves. If these valves malfunction or fail, blood pools in the veins rather than circulating out of the scrotum. This backup causes the veins to dilate and swell.
Why the Left Side?
Varicoceles occur on the left side about 85–90% of the time. This is due to the anatomical “path of least resistance.” The left testicular vein enters the renal vein at a perpendicular angle, making it harder for blood to flow upward compared to the right side, which enters the vena cava at a more direct angle.
Genetics
While there are no lifestyle-specific risk factors (like diet or exercise), genetics play a significant role. If your father or brother has had a varicocele, you are more likely to develop one.
The Link Between Varicoceles and Infertility
Perhaps the most significant complication of a varicocele is its impact on male infertility. Varicoceles are the most common identifiable cause of male factor infertility.
How it Affects Sperm
The primary function of the pampiniform plexus is to act as a heat exchanger, cooling the blood in the testicular artery before it reaches the testicles. Testicles must remain about 2°C to 3°C cooler than the rest of the body to produce healthy sperm.
When blood pools in a varicocele, the testicles overheat. This thermal stress leads to:
Decreased Sperm Count: Lower quantity of sperm produced.
Poor Motility: Sperm that cannot swim effectively.
Oxidative Stress: Damage to the sperm’s DNA.
Lower Testosterone: Reduced hormone production over time.
While approximately 40% of men with fertility problems have a varicocele, it is important to note that not all men with varicoceles are infertile.
Diagnosis and Testing
A diagnosis is usually reached through a simple physical examination. A doctor will feel the scrotum while you are standing and lying down.
In most cases, an ultrasound is not necessary for a diagnosis unless the physical exam is inconclusive or if the doctor needs to rule out other causes of scrotal pain. If fertility is a concern, a semen analysis is typically ordered to check for abnormalities in sperm count and quality.
Treatment Options: Is Surgery Necessary?
Treatment is not always required. If you are not experiencing pain and your fertility is not an issue, many doctors recommend “watchful waiting.” However, if a varicocele is causing discomfort or affecting your ability to conceive, several effective treatments exist.
1. Microsurgical Subinguinal Varicocelectomy
Considered the “gold standard,” this procedure uses a high-powered surgical microscope to identify and tie off the enlarged veins while preserving the delicate arteries and lymphatic vessels. It has the highest success rate and the lowest risk of complications.
2. Laparoscopic Surgery
The surgeon inserts a camera and small instruments through tiny incisions in the abdomen to clip the problematic veins.
3. Percutaneous Embolization
A less invasive option performed by a radiologist. A small catheter is inserted into a vein (usually in the groin or neck), and coils or fluids are used to block the blood flow to the varicocele, diverting it to healthy veins.
4. Open Surgery
A traditional surgical approach involving a larger incision to access the veins directly.
Recovery and Success Rates
The prognosis for varicocele repair is generally excellent:
Pain Relief: For those suffering from chronic aching, surgery is successful in 80% to 90% of cases.
Fertility Improvement: Approximately 70% of men see a significant improvement in sperm quality and quantity within 3 to 6 months of the procedure.
Assisted Reproduction: Repairing a varicocele can also increase the success rates of treatments like IVF (In Vitro Fertilization) and IUI (Intrauterine Insemination).
Summary Table: Varicocele Quick Facts
| Feature | Details |
| Prevalence | Affects 20% of the male population |
| Common Side | 90% occur on the Left Side |
| Primary Symptom | “Bag of worms” sensation or dull ache |
| Major Risk | Infertility (overheating of the testicles) |
| Gold Standard Cure | Microsurgical Varicocelectomy |
| Sperm Recovery | Improvements seen in 3–6 months post-surgery |
Conclusion
Varicoceles are a common biological occurrence, but they don’t have to define your reproductive future. Whether you are dealing with scrotal discomfort or navigating a difficult fertility journey, a varicocele is a highly treatable condition. By consulting with a urologist or a male infertility specialist, you can determine the best path forward to restore testicular health and improve your chances of starting a family.