Osteoporosis is often referred to as a “silent disease,” but its impact on global health is anything but quiet. As a condition characterized by weakened bones and a heightened risk of fractures, it remains a primary concern for aging populations.
Worldwide, 1 in 3 women and 1 in 5 men over the age of 50 will experience an osteoporotic fracture in their lifetime. Because the disease often progresses without symptoms until a break occurs, understanding your risk factors and the latest screening guidelines is essential for long-term mobility and health.
What is Osteoporosis?
Osteoporosis is a bone disease that develops when bone mineral density (BMD) and bone mass decrease, or when the structure and strength of the bone tissue change. This leads to fragile bones that are susceptible to fractures—even from minor stresses like coughing, bending over, or a fall from standing height.
While fractures can occur in any part of the skeleton, they are most common in the:
Hip
Spine (Vertebrae)
Wrist
Shoulder and Pelvis
The Critical Nature of Hip Fractures
In 2019 alone, approximately 14 million adults aged 50 and older sustained a hip fracture. This is considered the most serious consequence of the disease; statistics show that roughly 24% of people with a hip fracture die within a year of the injury due to complications and the resulting loss of mobility.
Symptoms: Why It Is Called a “Silent Disease”
Most people with osteoporosis have no idea they have it. There is no “feeling” of bones thinning. Often, the first sign is a painful fracture. However, some patients may notice physical changes if the vertebrae in the spine begin to weaken:
Severe back pain: Caused by a fractured or collapsed vertebra.
Loss of height: Over time, spinal compression leads to getting shorter.
Stooped posture: Also known as kyphosis or a “dowager’s hump,” resulting from the curvature of the upper spine.
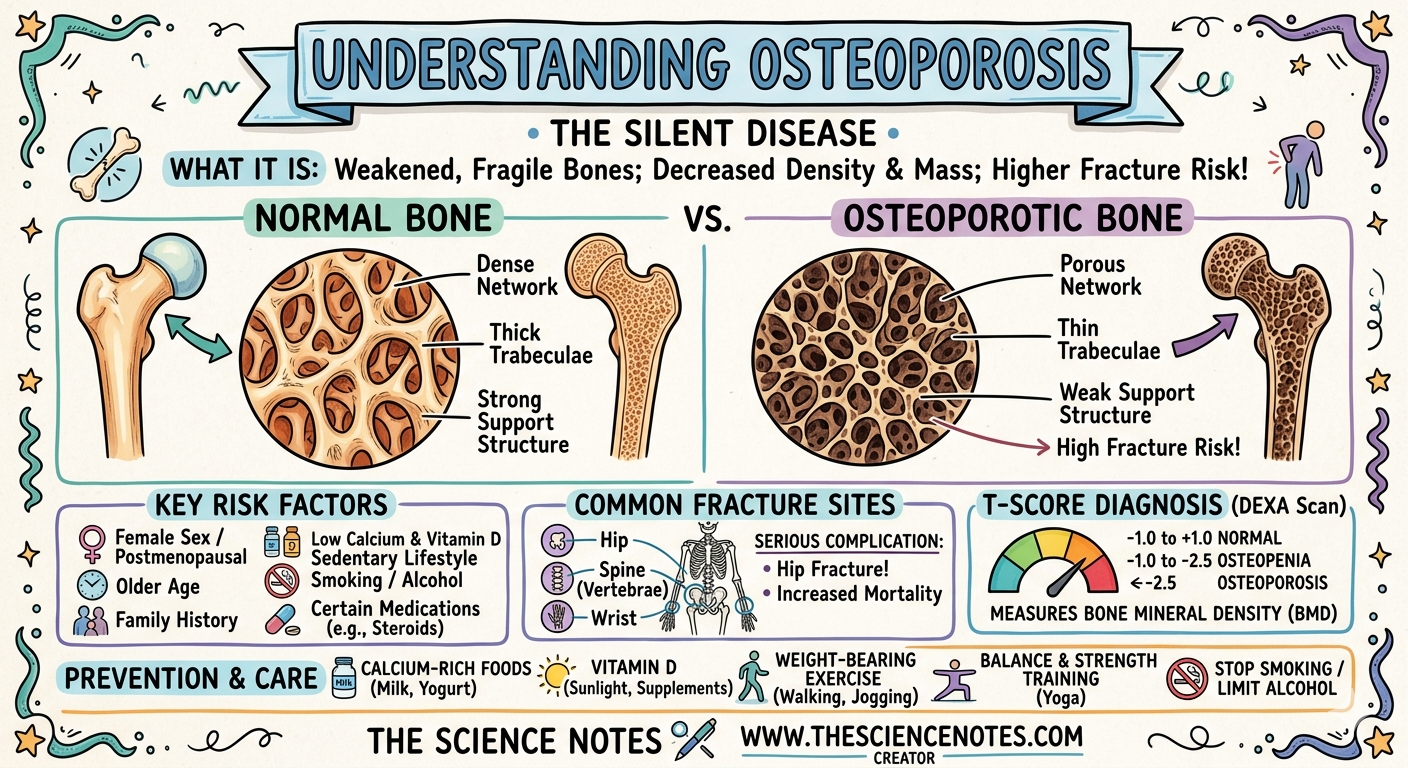
Risk Factors: Who Is Most at Risk?
Your risk for osteoporosis is determined by a combination of genetics, medical history, and lifestyle choices. Some factors are “non-modifiable” (you cannot change them), while others are within your control.
Non-Modifiable Risk Factors
Sex: Women are at higher risk because they have lower peak bone mass and smaller bones than men.
Age: Bone loss accelerates as you age, while new bone growth slows down.
Body Size: Small, slender individuals have less “reserve” bone mass to lose.
Race: The disease is most common among non-Hispanic white and Asian women. While African American and Hispanic women have lower statistically recorded risks, they remain significantly vulnerable.
Family History: Having a parent who suffered a hip fracture is a major predictor of your own bone health.
Hormonal Factors
Hormone imbalances significantly impact bone density:
Women: A drop in estrogen during menopause (especially before age 40) is a leading cause of bone loss.
Men: Low testosterone levels can weaken bones, though the gradual age-related decline is less of a factor than specific medical conditions causing low testosterone.
Medical Conditions and Medications
Certain diseases like Inflammatory Bowel Disease (IBD), Rheumatoid Arthritis, and Chronic Kidney Disease increase risk. Furthermore, long-term use of certain medications can leach minerals from the bone, including:
Glucocorticoids (Prednisone)
Antiepileptic drugs
Proton pump inhibitors (for stomach acid)
SSRIs (for depression)
Screening and Diagnosis: The T-Score Explained
Early detection is the key to preventing life-altering fractures. The medical gold standard for diagnosis is the DEXA (Dual-energy X-ray Absorptiometry) scan.
What is a DEXA Scan?
A DEXA scan is a low-dose X-ray that measures the calcium and mineral content in your bones. The result is typically reported as a T-score, which compares your bone density to that of a healthy young adult.
| T-Score | Meaning |
| -1.0 or higher | Normal bone density |
| Between -1.0 and -2.5 | Osteopenia (Low bone mass) |
| -2.5 or lower | Osteoporosis |
The FRAX Tool
Doctors also use the Fracture Risk Assessment Tool (FRAX). This algorithm combines your DEXA results with your personal risk factors (age, smoking status, etc.) to predict your percentage chance of having a major fracture in the next 10 years.
2025 Screening Guidelines: When Should You Get Tested?
According to the US Preventive Services Task Force (USPSTF) updated 2025 recommendations:
Women 65+: All women should be screened.
Women under 65: Screening is recommended for postmenopausal women who have an increased risk of osteoporosis as determined by a clinical risk assessment tool.
Men: Currently, the USPSTF states there is insufficient evidence to mandate universal screening for men, though many clinicians recommend it for men over 70 or those with significant risk factors.
Treatment Options: Medications for Bone Health
If you are diagnosed with osteoporosis, your doctor may prescribe one of two main types of medication:
1. Antiresorptive Drugs
These medications, including bisphosphonates and denosumab, work by slowing down the natural breakdown of bone tissue.
Note: Patients may sometimes take a “drug holiday” after 3 to 5 years of bisphosphonates to reduce the rare risk of jaw bone deterioration or unusual thigh bone fractures.
2. Anabolic Medications
Drugs such as teriparatide, abaloparatide, and romosozumab actually stimulate new bone formation. These are typically reserved for patients with severe osteoporosis or those who have already suffered multiple fractures.
Prevention: How to Build Stronger Bones
It is never too early—or too late—to start protecting your bone density. A proactive approach involves nutrition, lifestyle changes, and exercise.
1. The Power of Nutrition
Calcium and Vitamin D are the building blocks of bone.
Calcium (1000–1200 mg daily): Found in cow’s milk, fortified plant milks (soy/oat), leafy greens, and sardines.
Vitamin D (600–800 IU daily): Found in fatty fish, eggs, and fortified orange juice. Vitamin D is essential because it helps your body actually absorb the calcium you eat.
2. Weight-Bearing Exercise
Bones are living tissue that gets stronger when stressed. Incorporate:
Weight-bearing exercises: Walking, jogging, and climbing stairs.
Resistance training: Lifting weights or using resistance bands.
Balance training: Yoga or Tai Chi to prevent falls.
3. Lifestyle Adjustments
Maintain a Healthy BMI: A BMI below 20 is a significant risk factor for bone loss.
Quit Smoking: Smoking interferes with bone-building cells.
Limit Alcohol: Excessive drinking (more than 2 drinks a day) interferes with the body’s calcium balance.
Summary: Taking Control of Your Bone Health
Osteoporosis may be a “silent” threat, but it is manageable and, in many cases, preventable. By understanding your T-score, optimizing your intake of Calcium and Vitamin D, and engaging in weight-bearing exercises, you can significantly reduce your risk of fractures.
If you are a woman over 65, or if you have any of the risk factors mentioned above, consult your healthcare provider about a DEXA scan. Protecting your bones today is the best way to ensure your independence and mobility tomorrow.
Frequently Asked Questions (FAQ)
Can children get osteoporosis?
Yes, though it is rare. A condition called idiopathic juvenile osteoporosis can affect children. Most recover without treatment, but medical supervision is necessary.
Is it ever too late to treat osteoporosis?
No. Even if you have already sustained a fracture, medications and lifestyle changes can help prevent future breaks and improve bone quality.
Does a high-protein diet help?
Yes. Adequate protein intake is vital for bone health, especially in older adults. However, it must be balanced with sufficient calcium and Vitamin D.
More information: https://www.niams.nih.gov/health-topics/osteoporosis