History of Phage Therapy
Phage therapy has a long history, dating back over a century when it was independently discovered by Frederick Twort and Félix d’Hérelle. Initially overshadowed by antibiotics, the rise of antibiotic-resistant bacteria has sparked renewed interest in phage therapy. Ongoing research and advancements in phage isolation and purification techniques have reestablished its potential as an alternative or complement to antibiotics.
What is Phage Therapy?
Phage therapy uses bacteriophages, viruses that target and infect bacteria, to combat bacterial infections. These phages can be administered topically, orally, or intravenously, specifically targeting the infecting bacteria and leaving human cells unharmed. By injecting their genetic material into bacterial cells, phages take over the bacterial machinery, replicate, and ultimately destroy the infected cells.
How does Phage Therapy work?
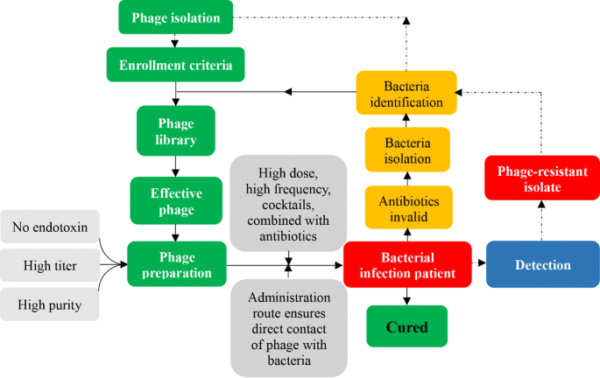
Phage identification:
Suitable phages are selected from a library to target the specific bacteria causing the infection.
Phage administration:
The chosen phages are administered to the patient, depending on the infection site and severity.
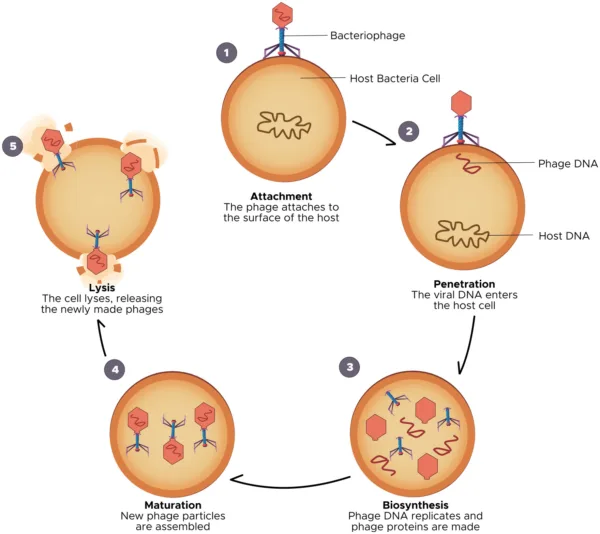
Phage attachment:
Phages bind to the target bacteria by attaching to receptors on the bacterial cell wall.
Phage penetration:
Phages inject their genetic material into bacterial cells, taking control of the bacterial machinery.
Phage replication:
Phage genes manipulate bacterial cells to produce more phages, resulting in thousands of new phages within each bacterium.
Bacterial lysis:
Accumulated phages cause the bacterial cell to burst, releasing more phages into the surrounding environment.
Bacterial clearance:
Released phages continue infecting and killing bacteria, reducing the infection’s bacterial population.
Specificity and selectivity:
Phages selectively target pathogenic bacteria while sparing beneficial bacteria and human cells.
Synergistic effects:
It can enhance the effectiveness of antibiotics against bacterial infections.
Treatment monitoring and adjustment:
Phage therapy is closely monitored, with phage selection and dosage adjusted as necessary for optimal outcomes.
Advantages and Disadvantages of Phage Therapy
Advantages:
- Targeted approach: Phage therapy specifically targets bacteria, minimizing harm to beneficial bacteria or human cells.
- Bacterial specificity: Phages can effectively combat antibiotic-resistant strains and target specific bacteria.
- Self-replication: Phages replicate within bacterial cells, leading to increased phage population and treatment effectiveness.
- Broad range of applications: It shows potential for treating various infections.
- Synergy with antibiotics: It can enhance the efficacy of antibiotics.
- Reduced side effects: Phages are generally well-tolerated and have a lower likelihood of adverse effects.
Disadvantages:
- Limited research and availability: Phage therapy is still under research and may not be widely accessible.
- Limited phage knowledge: Identifying appropriate phages for specific infections can be challenging.
- Potential immune response: Immune recognition of phages may reduce their effectiveness.
- Safety concerns: Phage-related side effects and safety profiles require further research.
- Development of phage resistance: Bacteria can develop resistance to phages over time.
- Regulatory challenges: Obtaining approvals for widespread use can be complex.
Applications of Phage Therapy
Phage therapy has emerged as a promising approach with diverse applications in treating bacterial infections. Here are some notable areas where phage therapy shows potential:
- Antibiotic-Resistant Infections: It offers an alternative for tackling antibiotic-resistant bacteria, which pose a significant challenge in healthcare settings.
- Chronic Wounds and Ulcers: Phage therapy can aid in the treatment of chronic wounds, such as diabetic foot ulcers or pressure ulcers, by targeting specific bacteria hindering the healing process.
- Respiratory Infections: Investigating bacteriophage therapy for respiratory infections caused by bacteria like Pseudomonas aeruginosa and Staphylococcus aureus, particularly in conditions such as cystic fibrosis and ventilator-associated pneumonia.
- Urinary Tract Infections: Bacteriophage therapy holds promise for addressing urinary tract infections (UTIs) caused by bacteria like Escherichia coli (E. coli) and Proteus mirabilis, offering targeted relief within the urinary tract.
- Gastrointestinal Infections: Exploring the potential of phage therapy for gastrointestinal infections caused by bacteria such as Salmonella, Shigella, and Clostridium difficile, while preserving the beneficial gut microbiota.
- Food Safety: Utilizing bacteriophage therapy to enhance food safety by selectively targeting and eliminating harmful bacteria in food products, reducing the risk of foodborne illnesses.
- Veterinary Medicine: Investigating bacteriophage therapy as an alternative to antibiotics in veterinary medicine, aiming to combat bacterial infections in farm animals and pets.
- Biofilm-Associated Infections: Addressing the challenges posed by bacterial biofilms, which exhibit increased resistance to antibiotics, by employing bacteriophage therapy to penetrate biofilms and disrupt bacterial populations within them.
Phage Therapy vs Antibiotics
Here is a table highlighting the key differences between Phage Therapy and Antibiotics:
| Aspect | Phage Therapy | Antibiotics |
| Target | Specific to bacteria | Broad spectrum |
| Mode of Action | Viral infection and lysis of bacteria | Inhibition of bacterial growth or killing |
| Specificity | Highly specific to target bacteria | Effective against various bacterial strains |
| Self-replication | Phages replicate within bacteria | Non-replicating chemical compounds |
| Natural entities | Naturally occurring viruses | Synthetic or derived from natural sources |
| Antibiotic Resistance | Potential efficacy against antibiotic-resistant strains | Can contribute to antibiotic resistance |
| Established Treatment | Emerging therapy with ongoing research | Well-established and widely used treatment |
| Synergy Potential | Can work synergistically with antibiotics | May be combined with other antibiotics for enhanced efficacy |
| Side Effects | Generally considered safe and well-tolerated | Can have side effects and impact beneficial bacteria |
| Prescription Availability | Limited availability, often on a case-by-case basis | Widely available and prescribed |
Future of Phage Therapy
- Advancements in Phage Discovery: Ongoing research expands knowledge of phages and identifies potent strains through improved isolation, characterization, and genetic engineering techniques.
- Optimal Formulation and Delivery: Researchers actively explore ideal methods for formulating and delivering bacteriophage therapy, including nanoparticle encapsulation and biomaterial-based carriers, to enhance stability, shelf life, and bioavailability during storage and transportation.
- Understanding Phage Pharmacokinetics and Pharmacodynamics: Studying phage behavior within the human body optimizes treatment effectiveness by examining distribution, elimination, and determining optimal dosing regimens.
- Synergistic Combination Therapies: By combining phage therapy with antibiotics or immune-based treatments, outcomes can be improved through the synergistic effects of tackling antibiotic resistance, persistent infections, and increasing overall success rates.
- Enhancing Phages for Improved Properties: Genetic engineering enables modifications to enhance phages, such as increased stability, broader host range, and improved bacterial killing mechanisms, effectively targeting resistance mechanisms and specific virulence factors.
- Rigorous Clinical Trials and Regulatory Approvals: Widespread adoption of bacteriophage therapy relies on comprehensive clinical trials and regulatory approvals, driving the development of standardized protocols and guidelines through collaboration between researchers, clinicians, and regulatory agencies.
- Personalized Medicine: The future of bacteriophage therapy lies in personalized treatment approaches, tailoring phages to specific bacterial infections to create personalized phage cocktails that maximize therapeutic efficacy and minimize resistance risks.
- Expanding Therapeutic Applications: Ongoing research may extend the scope of bacteriophage therapy beyond bacterial infections, enabling the targeting of other pathogens such as viruses and fungi, thereby offering potential treatments for a broader range of infectious diseases.
- Public Awareness and Acceptance: Raising awareness and educating healthcare professionals, patients, and the general public about bacteriophage therapy is crucial for its integration into mainstream healthcare. Increased awareness, funding, and public support foster further research, investment, and development of bacteriophage therapy.
References:
- Chanishvili, N. (2012). A Literature Review of the Practical Application of Bacteriophage Research. Journal of Microbiology, Epidemiology, and Immunobiology, 6-8.
- Cisek, A. A., & Dąbrowska, I. (2019). Gregor Mendel’s studies of bacteria: Relevance in the contemporary bacteriophage therapy. Frontiers in Microbiology, 10, 1008. doi: 10.3389/fmicb.2019.01008
- Pirnay, J.-P., et al. (2011). The Bacteriophage Therapy Paradigm: Prêt-à-Porter or Sur-mesure? Pharmaceutical Research, 28(4), 934-937. doi: 10.1007/s11095-010-0313-5
- Abedon, S. T., et al. (2011). Bacteriophage therapy pharmacology. Current Pharmaceutical Biotechnology, 12(8), 1319-1330. doi: 10.2174/138920111798357426
- Pires, D. P., et al. (2020). Understanding the Phag Therapy: Part of the Team. Antibiotics, 9(4), 293. doi: 10.3390/antibiotics9050293
- Golkar, Z., et al. (2014). Bacteriophage Therapy: A New Horizon in the Antibacterial Treatment of Oral Pathogens. Journal of Dental Research, Dental Clinics, Dental Prospects, 8(1), 1-6. doi: 10.5681/joddd.2014.001
- Roach, D. R., et al. (2017). Bacteriophage Therapy Faces Evolutionary Challenges. Viruses, 9(10), 290. doi: 10.3390/v9100290
- Górski, A., et al. (2020). Phages and Immunomodulation. Future Microbiology, 15(1), 1375-1377. doi: 10.2217/fmb-2020-0090
- Sulakvelidze, A., et al. (2001). Bacteriophage Therapy. Antimicrobial Agents and Chemotherapy, 45(3), 649-659. doi: 10.1128/AAC.45.3.649-659.2001
- Jennes, S., et al. (2017). Bacteriophages: An Alternative to Conventional Antibiotics in Clinical Practice? Pharmacy, 5(4), 6. doi: 10.3390/pharmacy5010006
Learn more