Introduction to Systemic Lupus Erythematosus (SLE)
Systemic Lupus Erythematosus (SLE), commonly known as lupus, is a chronic autoimmune condition that impacts different parts of the body. This disorder occurs when the immune system mistakenly attacks its own tissues, leading to inflammation and potential harm to organs and systems. With a complex array of symptoms and potential complications, lupus presents unique challenges for diagnosis and management.
Symptoms and Presentation of Systemic Lupus Erythematosus
Lupus manifests through a diverse range of symptoms, which can differ significantly from person to person. Frequent symptoms encompass fatigue, joint discomfort, skin rashes, fevers, and swelling. Multiple organ systems, including the skin, joints, heart, lungs, kidneys, blood vessels, and brain, can be affected. Notable symptoms include:
- Skin rashes, including the characteristic “butterfly” rash across the nose and cheeks.
- Joint pain and swelling, resembling arthritis.
- Persistent fatigue and low-grade fevers.
- Sunlight sensitivity leading to skin rashes.
- Kidney damage causing alterations in kidney function and potential kidney failure.
- Heart-related issues such as heart muscle or valve inflammation.
- Neurological symptoms like headaches, confusion, and seizures.
- Blood clotting irregularities increasing the risk of clot-related complications.
- Abnormalities in blood cell counts.
- Inflammation of the lungs and lung lining.
- Gastrointestinal symptoms, including abdominal pain.
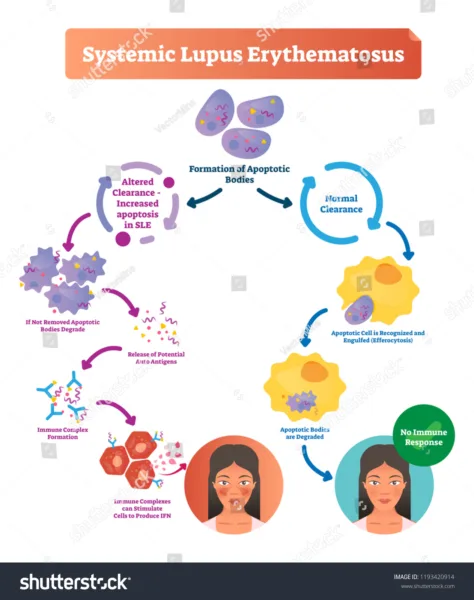
Causes and Risk Factors of Systemic Lupus Erythematosus:
- Unknown Cause: While the precise cause of lupus is unidentified, it’s believed to result from a combination of genetic, environmental, and hormonal factors.
- Gender and Age: Women, particularly in their childbearing years, are more susceptible to lupus than men. Prevalence is often higher in women aged 15 to 44 due to hormonal influences.
- Ethnicity: Certain ethnic groups, such as African Americans, Asians, and Hispanics, exhibit a higher occurrence of lupus. Genetics, including a family history of autoimmune diseases, can elevate risk.
- Genetic Predisposition: Genetic factors contribute to lupus development, as the immune system erroneously targets healthy tissue.
- Environmental Triggers: Factors like sunlight, infections, medications, and stress can trigger lupus in genetically predisposed individuals.
- Sunlight: Sun exposure can induce lupus skin lesions or internal responses in those with a genetic predisposition.
- Infections: Infections may initiate lupus or cause relapses in certain individuals.
- Medications: Specific medications, like blood pressure drugs and antibiotics, can trigger drug-induced lupus, with symptoms usually improving upon medication cessation.
Risk Factors:
- Sex: Lupus is more common among females.
- Age: Onset typically occurs between 15 and 45 years old.
- Race: African Americans, Hispanics, and Asian Americans face higher risks.
- Genetics and Hormones: Genetic inclination and hormonal changes, like those during puberty, contribute to susceptibility.
- Sunlight Exposure: Increased sunlight exposure heightens lupus risk.
- Smoking: Smoking may raise the risk of lupus.
- Medications: Certain drugs can lead to drug-induced lupus, with symptoms generally abating after discontinuation.
- Family History: A family history of lupus increases the likelihood of developing the condition.
- Non-Contagious: Lupus is not transmissible between individuals.
Diagnosis of Systemic Lupus Erythematosus
Diagnosing SLE involves intricate clinical insights, cytopenias, and autoantibodies:
- Clinical Criteria: Suspect SLE in individuals, particularly young women, exhibiting symptoms aligned with the disease. Differentiating early-stage SLE from other disorders like rheumatoid arthritis is crucial. Conditions like infections can also mimic SLE, especially in immunosuppressed patients.
- Laboratory Testing: Essential tests include antinuclear antibodies (ANA) and anti-double-stranded (ds) DNA tests, complete blood count (CBC), urinalysis, and a chemistry profile including renal and liver enzymes.
- EULAR/ACR Classification Criteria: Rely on the EULAR/ACR criteria for SLE diagnosis, which consider clinical and immunologic domains. A positive ANA ≥ 1:80 is a prerequisite. A score of 10 or more, along with fulfilling at least one clinical criterion, classifies as SLE.
- Fluorescent ANA Test: This sensitive test is pivotal. Positive ANA tests, often at high titer (>1:80), are found in over 98% of SLE cases. However, they can occur in other conditions as well, necessitating careful interpretation.
- Autoantibodies: Evidence of specific autoantibodies aids diagnosis. Some are specific to certain manifestations, such as anti-Ro for neonatal lupus.
Monitoring Severity:
Monitoring extends beyond diagnosis:
- Parameters like serum complement levels, ESR, and C-reactive protein offer insight into disease activity.
- Regular urinalysis detects kidney involvement, even in seemingly asymptomatic cases.
Treatment of Systemic Lupus Erythematosus:
- Individualized Approach: Treatment is personalized based on disease severity and symptoms.
- Medications: Management involves various drug groups addressing different aspects.
- NSAIDs: Non-steroidal anti-inflammatory drugs alleviate inflammation and pain.
- Antimalarials: These control joint pain, skin rashes, and fatigue while lowering cholesterol.
- Corticosteroids: Potent anti-inflammatory corticosteroids manage serious complications affecting the heart, lungs, and nervous system.
- Immunosuppressants: Immune-suppressing drugs like methotrexate control immune responses.
- Cytotoxic Drugs: These are reserved for severe manifestations, especially kidney inflammation.
- Collaborative Care: Rheumatologists and specialists collaborate for accurate diagnosis, effective treatment, and ongoing monitoring.
- Tailored Plans: Customized plans ensure symptom control and quality of life.
- Long-Term Monitoring: Regular follow-ups evaluate treatment effectiveness.
The primary goals are symptom management, flare-up prevention, and minimizing organ damage. Lifestyle adjustments like stress management and exercise complement medications.
Living with Lupus:
Active management involves personalized plans, monitoring, medication adjustments, and lifestyle changes. A balanced diet, exercise, and stress management are key.
Pregnancy and Contraception:
Consulting healthcare providers is crucial for healthy pregnancies. Some medications may need adjustments. Birth control options should consider factors like antiphospholipid antibodies.
Conclusion:
SLE is intricate but manageable with early diagnosis, personalized treatment, and healthy choices. Collaboration with healthcare providers empowers patients to live well with lupus.
Learn more
Blood Tests: Types, Normal Ranges, and Abnormal Indications (thesciencenotes.com)
References
- Centers for Disease Control and Prevention (CDC). (n.d.). Lupus: Detailed Fact Sheet. Retrieved from source
- MedlinePlus. (2021). Lupus. Retrieved from source
- National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS). (n.d.). Lupus. Retrieved from source
- Cleveland Clinic. (n.d.). Lupus. Retrieved from source
- Mayo Clinic. (2021). Lupus. Retrieved from source
- NHS. (2021). Lupus. Retrieved from source
- Medical News Today. (2022). Lupus: Causes, Symptoms, and Treatment. Retrieved from source
- Nature Reviews Drug Discovery. (2017). Lupus: Advances in Treatment and Understanding the Disease. Retrieved from source