Blood is a fluid that circulates continuously and carries nutrients, oxygen, and waste out of the body. Since most of blood is liquid and contains countless suspended cells and proteins, blood is “thicker” than pure water. Strongly stated, blood is a living tissue made up of cells suspended in a fluid “matrix,” not a bodily fluid like tear, mucus, saliva, urine, or sweat. Blood’s primary purpose is to maintain a fluid balance throughout the body. The average person’s blood volume is roughly 4.8 (4-5) liters, or around 7- 8% of their body weight. Blood loss of 15% to 30% induces pallor and weakness. If more than 30% of blood is lost, severe shock and death of the person result.
Components of Blood
Four main constituents of Blood are:
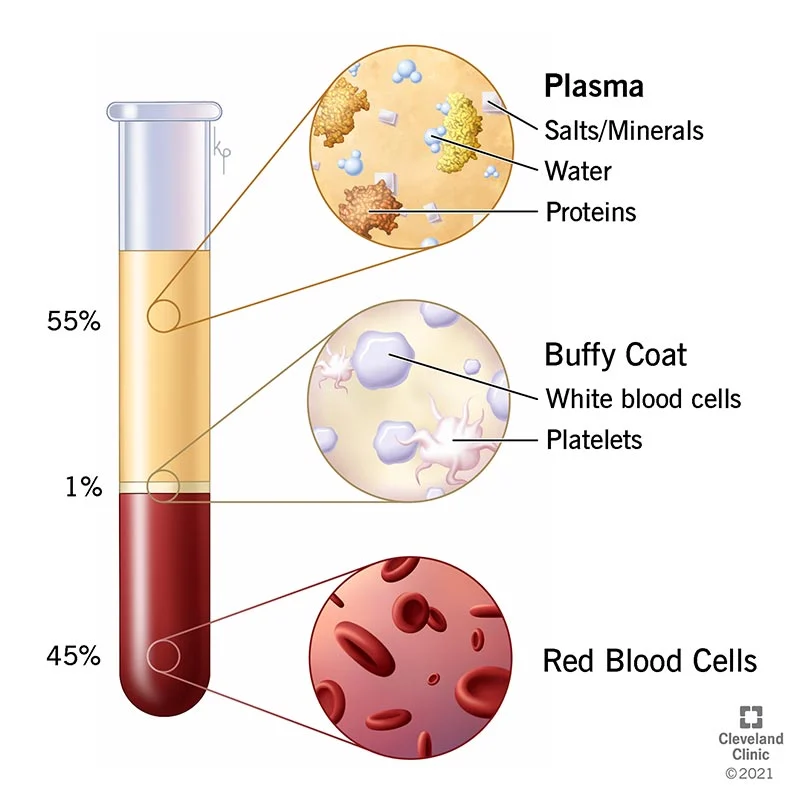
Plasma, Red blood cells (RBC), White blood cells (WBC), and Platelets. Plasma makes up 55% of the blood, with blood cells making up the remaining 45%.
What is Blood Plasma?
Blood plasma, often known as plasma, has a straw-colored or pale-yellow appearance. It acts as entire blood’s liquid foundation. The greatest component of your blood is called plasma. It accounts for more than half (about 55%) of the entire content. The primary function of plasma is to carry blood cells, as well as nutrients, waste products, antibodies, clotting proteins, chemical messengers like hormones, and proteins that support the body’s fluid balance, throughout the body.
Where is plasma made?
Plasma cells are created in the embryo by cells in your umbilical cord. In the soft tissue of your bones (bone marrow), liver cells, blood cells at the end of their lives, and your spleen, plasma proteins grow after development.
Centrifugation, or spinning whole blood with an anticoagulant in a centrifuge, is a technique that can be used to separate it from whole blood. The yellow, top layer is plasma and the bottom layer contains your blood cells (red and white) and platelets. To preserve the functionality of the various clotting factors and immunoglobulins, the plasma is collected and frozen within 24 hours. It is thawed before usage and has a shelf life of one year. Interestingly, AB blood group plasma is the most favored because it does not contain antibodies, making it appropriate for everyone without concern of an adverse reaction, although O- blood group is the chosen universal donor for blood.
The following are signs of plasma conditions:
- bone ache.
- easily bleeding or bruising.
- heart flutters (arrhythmia).
- Having wrist and hand pain (carpal tunnel syndrome).
- compromised immune system
Red Blood Cells (RBC/ Erythrocytes)
Red blood cells have a biconcave disk shape with a flattened center, which means that both of the disc’s faces have shallow bowl-shaped indentations (a red blood cell looks like a donut).
Red blood cells are more malleable when they lack a nucleus, but their lifespan is also shortened. Haemoglobin, a protein found in red blood cells, aids in the transfer of oxygen from the lungs to the body’s tissues and then helps the body return carbon dioxide to the lungs. Hematocrit, a commonly used indicator of red blood cell levels, is the percentage of total blood volume made up of red blood cells. In terms of hematocrit, men typically have values between 44 and 45 percent of blood volume, whereas women typically have values between 39 and 44 percent of blood volume.
How is RBC produced?
Erythropoietin, a hormone mostly generated by the kidneys, regulates the production of red blood cells. In the bone marrow, red blood cells begin as immature cells and mature over the course of about seven days before being discharged into the bloodstream. Red blood cells can quickly alter shape and, in contrast to many other cells, lack a nucleus, which helps them pass through the body’s numerous blood channels. While a red blood cell’s lack of a nucleus makes it more flexible, it also shortens the cell’s lifespan as it passes through the tiny blood channels, harming its membranes and wasting its energy reserves. The average lifespan of a red blood cell is only 120 days.
Disorders of Erythrocytes
Polycythemias and anemias are erythrocyte diseases. A set of disorders known as anemias show symptoms including a reduced ability of the blood to transport oxygen. They are mostly brought on by either a decline in erythrocyte count or a decline in hemoglobin content within RBCs. Anemia causes tissues to get insufficient oxygen delivery, which manifests as pallor, weariness, shortness of breath, and lightheadedness.
A disease known as polycythemia, which is characterized by an increased RBC count, is the reverse of anemia. It is substantially less common than anemias.
White Blood Cells (WBC/ Leukocytes)
Leukocytes, also known as white blood cells or leukemia cells, are immune system components that take part in both innate and humoral immune responses. In Greek, leucko means white and cyte means cell.
They circulate through our bloodstream to defend against bacteria, viruses, and other harmful foreign invaders. White blood cells rush to the scene when our body is in crisis and a specific location is being attacked in order to assist in destroying the pathogen and avert sickness. Just 1% of our blood is made up of white blood cells.
How are white blood cells formed?
White blood cells develop from stem cells, or cells that can change into various types of cells in the body, in the soft tissue of your bones (bone marrow). The soft tissue inside the bones is where white blood cell production takes place (bone marrow). The lymph nodes, spleen, thymus gland, and T cells all contain two different types of white blood cells called lymphocytes (B cells). The average lifespan of WBC is 13 to 20 days, after which they are destroyed in lymphatic system.
Types of white blood cells
White blood cells come in five different varieties:
- Neutrophils: Eradicates bacteria, fungus, and foreign debris, they assist in defending our body against illnesses.
- Lymphocytes: It consists of T cells, natural killer cells, and B cells make up lymphocytes, which protect against viral infections and create proteins that aid in infection defense ( antibodies).
- Eosinophils: Can recognize and kill parasites and cancer cells; and Help basophils with allergic reaction
- Basophils: Causes allergic reactions such as runny nose, coughing, and sneezing.
- Monocytes: Clear away harmed cells to protect against infection.
Disorders that affect WBC
Infections are more likely to affect people if the white blood cell count is low (leukopenia). Leukocytosis, or an excessively high white blood cell count, may indicate an underlying illness such leukemia, lymphoma, or an immunological problem.
Platelets (Thrombocytes)
Platelets are a little, disc-shaped cell fragment that can be discovered in the spleen and blood. Megakaryocytes, very big cells found in the bone marrow, are the building blocks of platelets. They aid in the formation of blood clots that help wounds heal and to slow or stop bleeding. Once platelets are made and circulated into your bloodstream, they live for 8 to 10 days.
What happens if you have a high or low platelet count?
Thrombocytopenia
The bone marrow produces insufficient platelets or platelets are damaged in this situation. If the platelet count becomes too low, bleeding may happen under the skin as a bruise, internally as internal bleeding, externally as a nosebleed or from a wound that won’t stop bleeding.
Thrombocytosis
Unknown factors contribute to an increase in platelets caused by abnormal bone marrow cells. It could be brought on by a chronic illness or condition like anemia, cancer, inflammation, or infection.
Typical range of Blood Components
| Components | Values and Ranges |
| White blood cell count (WBC) | 4,300 to 10,800 cells per cubic millimeter |
| White blood cell (WBC) differential count | The cells in a differential count are granulocytes, lymphocytes, monocytes, eosinophils, and basophils |
| Red cell count (RBC) | 4.2 to 5.9 million cells/cubic millimeter |
| Platelet count | 150,000 to 400,000 / cubic millimeter |
Functions of Blood
The main role of blood is to keep the internal conditions of our body stable. The blood flowing through the veins, tolerance to dietary and fluid changes, and resistance to physical harm, chemical toxins, and infectious pathogens. Furthermore, blood contribute to the body’s capacity to adapt to changing life circumstances, such as the ability to withstand significant changes in climate and air pressure and the capacity to alter the amount of physical activity.
Blood has some critical functions, such as:
- Fluid connective tissue
- Transporting nutrition and oxygen to the tissues, including the lungs and remove carbon dioxide
- Clotting blood to stop excessive blood loss; A clot is formed at the site of the wound by the interaction of platelets and fibrin.
- Transporting immune system cells and antibodies. WBC are the disease fighting component of blood. White blood cells can be classified into five different groups: neutrophils, eosinophils, basophils, lymphocytes, and monocytes. The majority of white blood cells, between 60% and 70%, are neutrophils.
- Transporting waste to the liver and kidneys, which filter and cleanse the blood. Renal arteries carry blood into the kidneys, and renal veins carry it out. The ureters receive the waste products that the kidneys remove from the blood plasma, including urea, uric acid, and creatinine. Blood poisons are also eliminated by the liver. It purifies vitamin-enriched blood during digestion before redistributing it to the rest of the body.
- Homeostasis: regulation of body temperature. When responding to internal hormone and chemical changes as well as to external organisms like bacteria, blood arteries dilate and constrict. These movements shift heat and blood toward or away from the skin’s surface, where heat is lost.
References
https://my.clevelandclinic.org/health/body/22865-plasma
https://www.ncbi.nlm.nih.gov/books/NBK531504/
https://www.visiblebody.com/learn/circulatory/circulatory-functions-of-the-blood
https://www.hematology.org/education/patients/blood-basic
https://www.kenhub.com/en/library/anatomy/erythrocytes
https://my.clevelandclinic.org/health/body/21871-white-blood-cells
https://www.urmc.rochester.edu/encyclopedia/content.aspx?ContentID=35&ContentTypeID=160