Understanding an individual’s blood group is a critical component of modern medicine. It ensures compatibility in blood transfusions, organ transplants, and even during pregnancy. Determining these blood groups involves the ABO and Rh blood typing systems, utilizing specific antigens and corresponding anti-sera to identify an individual’s unique biological marker.
What is Blood Typing?
Blood typing is a laboratory procedure used to determine a person’s blood group based on the specific antigens—protein molecules—present on the surface of their red blood cells (RBCs). These antigens serve as the foundation for blood grouping and are recognized by the immune system.
The two primary systems used in clinical practice are:
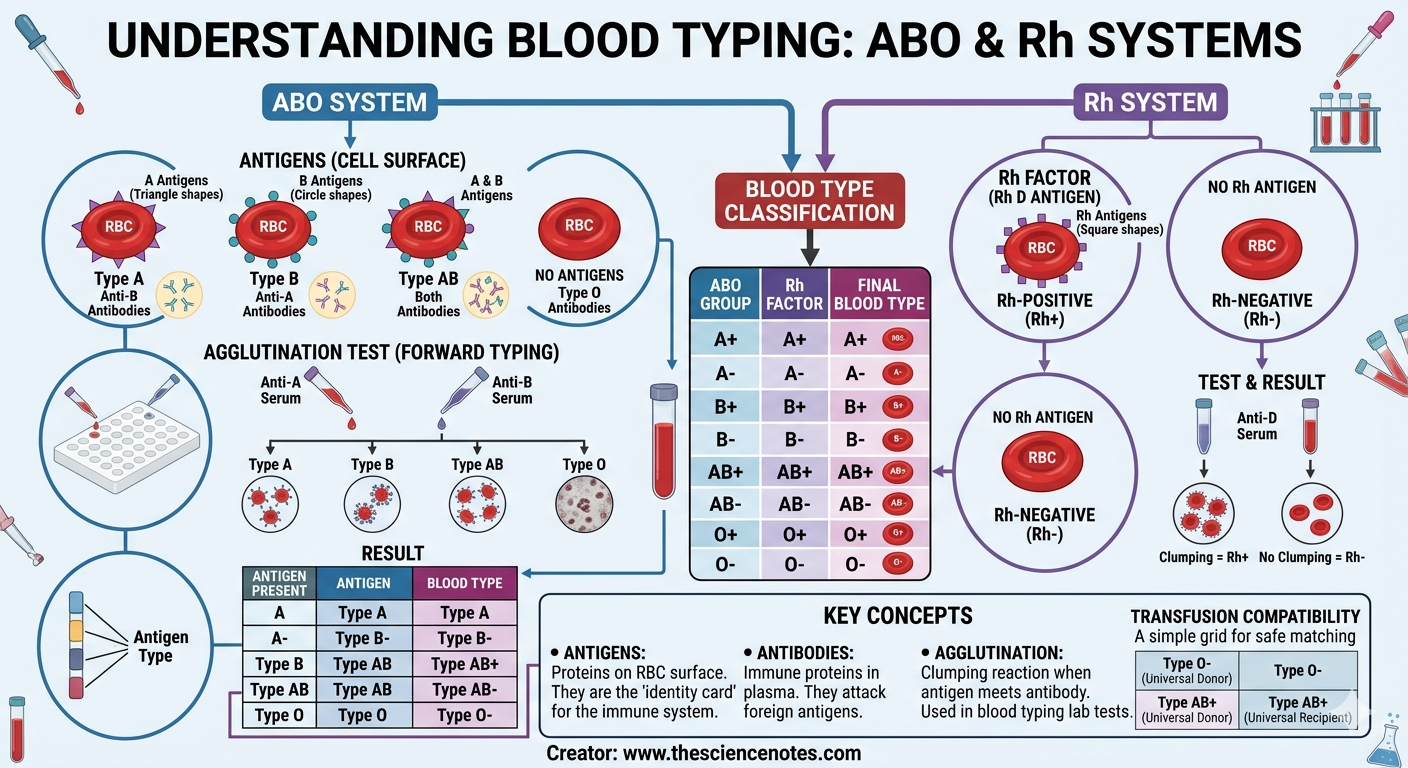
ABO System: Classifies blood into four types (A, B, AB, and O) based on the presence or absence of A and B antigens.
Rh System: Categorizes blood as Rh-positive or Rh-negative, depending on the presence of the Rh D antigen.
Discovered in 1901 by Karl Landsteiner, blood typing has become a cornerstone of patient safety. It allows healthcare providers to manage everything from emergency trauma to maternal-fetal health with high precision.
The Importance of Blood Typing in Health and Medicine
The accuracy of blood typing impacts four major areas of healthcare and the pharmaceutical industry.
1. Safe Blood Transfusions
In transfusion medicine, accurate typing prevents hemolytic transfusion reactions. This occurs when a recipient’s immune system attacks mismatched donor blood, leading to the rapid destruction of red blood cells. Such reactions are life-threatening and are most commonly caused by clerical errors or incorrect typing. In emergency settings, understanding the “Universal Donor” status of O-negative blood is a literal life-saver.
2. Pregnancy and Prenatal Care
Identifying the Rh factor is vital for preventing Rh incompatibility. If a pregnant mother is Rh-negative and the fetus is Rh-positive, the mother’s immune system may produce antibodies that attack the baby’s red blood cells. This can lead to hemolytic disease of the newborn (HDN). Fortunately, doctors can administer Rh immune globulin (RhoGAM) to prevent this immune response, a discovery that has saved countless infant lives.
3. Organ and Bone Marrow Transplantation
Successful transplants require close matching of ABO and Rh types. Compatibility reduces the risk of hyperacute rejection, where the body rejects a new organ within minutes or hours. Proper matching improves long-term survival rates for patients receiving kidneys, hearts, or stem cells.
4. Pharmaceutical and Biologic Manufacturing
In the industrial sector, blood typing ensures the safety of plasma-derived products and cell therapies. It is essential for the development of IVIG (Intravenous Immunoglobulin) therapies and other medications derived from human plasma under strict GMP (Good Manufacturing Practice) conditions.
The Science of Antigens and Agglutination
The identification of blood groups relies on a biological process known as agglutination.
What are Antigens?
Antigens are protein or sugar molecules residing on the surface of red blood cells. The ABO and Rh systems specifically target:
Antigen A
Antigen B
Antigen D (Rh)
These antigens are generated by reactions catalyzed by enzymes called glycosyltransferases. The human ABO gene, located on chromosome 9, determines which antigens your body produces.
The Agglutination Reaction
Agglutination is a reaction that occurs when an antigen comes into contact with its corresponding antibody, causing the cells to clump together. In a lab setting, technicians use “anti-sera” (solutions containing known antibodies) to trigger this reaction and identify the blood type.
| Anti-Serum | Target Antigen | Purpose |
| Anti-A Serum | Antigen A | Identifies Type A or AB |
| Anti-B Serum | Antigen B | Identifies Type B or AB |
| Anti-D Serum | Rh (D) Antigen | Determines Rh-positive/negative status |
Comprehensive Classification of Blood Types
Blood types are inherited and determined by the ABO gene on chromosome 9 and the RHD gene on chromosome 1.
The ABO Blood Group System
Type A: Has A antigens on the RBCs and produces anti-B antibodies in the plasma. Type A individuals can receive A and O type blood.
Type B: Has B antigens and anti-A antibodies. They can receive B and O blood types.
Type AB: Has both A and B antigens and no antibodies in the plasma. This makes Type AB the universal recipient for red blood cell transfusions.
Type O: Lacks both A and B antigens but has both anti-A and anti-B antibodies. It is the universal donor for red blood cells.
The Rh Factor Classification
In addition to the ABO group, blood is classified by the Rh factor:
Rh-positive (Rh+): Red blood cells carry the Rh D antigen. Roughly 85% of the population is Rh-positive.
Rh-negative (Rh-): Red blood cells lack the Rh D antigen.
Combining these systems results in the eight common blood types: A+, A-, B+, B-, AB+, AB-, O+, and O-.
Step-by-Step Laboratory Process of Blood Typing
Determining a blood group involves a standardized five-step process performed under regulated laboratory conditions to ensure 100% accuracy.
Step 1: Sample Collection
A small blood sample is drawn, usually from a vein (venipuncture) or a finger prick (peripheral blood). The sample is collected into tubes containing anticoagulants like EDTA to prevent clumping before the test begins.
Step 2: Forward Typing (Cell Typing)
The patient’s red blood cells are mixed with commercial Anti-A and Anti-B sera.
If agglutination (clumping) occurs with Anti-A, the patient has the A antigen.
If it clumps with Anti-B, they have the B antigen.
If it clumps with both, they are Type AB.
Step 3: Reverse Typing (Serum Typing)
To confirm the results, the patient’s serum or plasma is tested against known Type A and Type B red blood cells.
A Type A person should have anti-B antibodies.
A Type O person should have both anti-A and anti-B antibodies.
This “double-check” ensures that the antigens on the cells match the antibodies in the plasma.
Step 4: Rh Typing
The sample is mixed with Anti-D antibodies. If the blood clumps, the individual is Rh-positive. If no reaction occurs, they are Rh-negative.
Step 5: Crossmatching (Compatibility Testing)
Immediately before a transfusion, the recipient’s serum is mixed with the specific donor’s red blood cells. This “final check” detects any unexpected antibodies that might have been missed in general typing, preventing acute hemolytic reactions.
Discrepancies and Rare Phenotypes
While blood typing is usually straightforward, certain clinical scenarios create discrepancies between forward and reverse typing.
1. Subgroups of A and B
Some individuals have “weak” expressions of antigens. For example, the A blood type has subgroups like A1 and A2. A2 individuals have fewer A antigens on their cell surfaces, which can sometimes lead to weaker agglutination in the lab.
2. Acquired B Phenomenon
This rare phenomenon occurs primarily in patients with colorectal cancer or intestinal obstructions. Certain bacteria release enzymes that chemically modify the “A” antigen so that it mimics a “B” antigen. In the lab, a Type A person might temporarily appear to be Type AB.
3. The Bombay Phenotype (hh)
The “H antigen” is the precursor molecule required to build A and B antigens. In extremely rare cases (mostly in parts of India), individuals lack this H antigen. They appear to be Type O in standard tests, but they carry a potent anti-H antibody. If a Bombay phenotype person receives standard Type O blood, they will have a severe reaction. They can only receive blood from other Bombay phenotype donors.
Clinical Significance: Transfusion and Emergency Care
Transfusion Guidelines
In the simplest terms, the goal is to avoid introducing an antigen that the recipient’s immune system will recognize as “foreign.”
| Recipient Type | Compatible RBC Donor | Compatible Plasma Donor |
| A | A, O | A, AB |
| B | B, O | B, AB |
| AB | All Types (Universal) | AB Only |
| O | O Only | All Types (Universal) |
Emergency “Flying Squad” Blood
In trauma situations where there is no time for a full crossmatch, hospitals use O-negative red blood cells and AB plasma (or low-titer O whole blood). Because O-negative cells have no A, B, or Rh antigens, they are the safest “blind” choice for any patient.
FAQs about Blood Typing
What is a universal blood donor?
Type O-negative (O-) is the universal donor. Its cells lack A, B, and Rh antigens, making it safe for almost anyone to receive in an emergency.
What is a universal blood recipient?
Type AB-positive (AB+) is the universal recipient. Since these individuals have all three antigens (A, B, and Rh), their immune system will not attack any donor blood type.
Can blood type change over time?
In 99.9% of cases, no. However, patients who undergo bone marrow or stem cell transplants may eventually take on the blood type of their donor as the new marrow begins producing blood cells.
Is blood type linked to disease?
Recent research suggests links between blood types and certain health risks. For example, Type O individuals may have a slightly lower risk of blood clots and cardiovascular disease, while non-O types may have different susceptibility levels to certain viral infections.
How accurate is blood typing?
When performed in a certified clinical laboratory using both forward and reverse typing, the accuracy is nearly 100%. Most errors are “clerical”—meaning they happen during labeling or data entry, rather than during the chemical test itself.
Conclusion: The Bridge Between Lab and Life
Blood typing is much more than a routine laboratory test; it is a life-saving diagnostic tool. It bridges the gap between complex molecular biology and clinical safety. From ensuring the success of a kidney transplant to protecting a newborn from hemolytic disease, the ABO and Rh systems remain fundamental to the medical industry.
By strictly following protocols for Forward Typing, Reverse Typing, and Crossmatching, healthcare teams can provide precise and effective care. Whether you are a patient, a student, or a healthcare professional, understanding the interaction between antigens and antibodies is key to appreciating the “silent” safety net of modern transfusion medicine.