Hematopoiesis is the process of blood cell development. Hematopoiesis is the lifetime process of ongoing blood cell production and turnover to satisfy both daily needs and to address elevated demands, such as those caused by injury or illness. The lifespan of mature blood cells is limited and needs to be continuously replenished by the formation of new blood cells.
Around one trillion blood cells, including 200 billion erythrocytes (Red blood cells, or RBCs) and 70 billion neutrophils, are produced daily by average human adults.
Hematopoiesis is derived from two Greek terms:
- Haîma: Blood.
- Poiēsis: To make something.
The terms hemopoiesis, hematogenesis, and hemogenesis are all used to refer to hematopoiesis.
Types of Blood cells
Hematopoiesis includes the making of all blood types, including Red Blood cells, White Blood cells and Platelets. The production of RBC, or Erythrocytes is called erythropoiesis. Similarly, the production of WBCs, or leukocytes is called leukopoiesis; and, the production of Platelets, or thrombocytes is called thrombopoiesis.
Learn more:
Functions and Components of Blood cells
Organ of Hematopoiesis
- According to the commonly recognized monophyletic hypothesis of hematopoiesis, all hematopoietic cells are produced from pluripotent stem cells that then develop into unipotent ones and precursor cells before producing adult blood cells.
- In humans, hematopoiesis starts in the yolk sac, momentarily moves to the liver, and then eventually establishes itself in the bone marrow and thymus.
When a human body is still in the uterus, hematopoiesis begins in the yolk sac, a structure that envelops an embryo at the beginning of pregnancy. The majority of blood cell production occurs in the bone marrow toward the ending of pregnancy.
- Week 3: The yolk sac produces a kind of red blood cell that is slightly less developed than the red blood cells that are produced throughout maturity.
- Weeks 2 and 3: Your liver and spleen produce platelets and red blood cells, respectively. Your liver, spleen, and thymus all produce white blood cells.
- Month 5: Your bone marrow produces the majority of your blood cells. Certain kinds of white blood cells are also made by the thymus, spleen, and other lymph tissue.
- After Birth : The bone marrow is where the majority of blood cells are made from infancy through maturity. Thymus also contributes to the development of certain lymphocyte subtypes of white blood cells.
Learn more:
Human Fetus development :
Source:
Process of Hematopoiesis
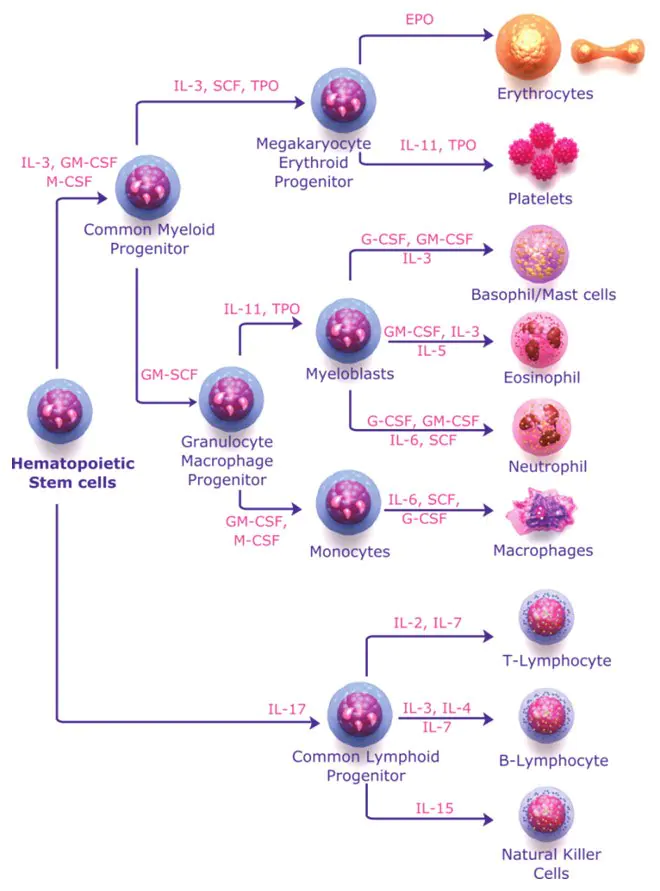
- An unspecialized stem cell initiates the hematopoiesis process. All the blood cells formed are derived from the common progenitor called as Hematopoietic stem cells, HSCs. The hematopoietic stem cell (HSC) sits at the pinnacle of hematopoiesis and is characterized by two fundamental properties: the capacity for multipotent differentiation into all mature blood lineages, including erythrocytes, platelets, lymphocytes, monocytes/macrophages, and granulocytes; and the capacity for self-renewal, a divisional event that produces two HSCs.
- HSCs differentiates into different progenitor cells which further differentiate to lymphoid or myeloid progenitor cells that leads to the production of various types of blood cells. It is a tightly regulated process, controlled by several growth factors and transcription factors. They regulate, self-renewal, proliferation, differentiation, and survival or death of the blood cells throughout the process of hematopoiesis.
- Common lymphoid progenitors (CLPs) or common myeloid progenitors are formed from multipotent progenitors(MPPs), which have a diminished ability for self-renewal (CMPs).
- Common lymphoid progenitor cells differentiate into lymphoid cells, whereas Common Myeloid progenitors differentiates into myeloid cells.
- Cytokine stimulation and transcription factor modulation are required for the commitment of hematopoietic cells to more lineage-restricted cells.
- Lymphoid progenitor cells differentiate into B cells, T cells and NK cells.
- Myeloid progenitor cells differentiate into Granulocyte-Monocyte progenitor cells, Erythrocyte progenitor, or Megakaryocyte progenitor cells. Granulocyte-Monocyte progenitor cells differentiate and develop into neutrophil, eosinophil or basophil; and monocyte develops into macrophages.
- Similarly, Erythrocyte progenitor cells and megakaryocyte progenitor cells give rise to erythrocytes (RBCs), and Megakaryocytes (Platelets), respectively.
Learn more:
Hierarchy of Cell potency
Regulation of Hematopoiesis
- The self-renewal and differentiation of HSCs is regulated by different growth factors and transcription factors and Stem cell Factors (SCFs).
- Many transcription factors control the number and stage of differentiation of stem cells. Hematopoietic cell fate is controlled by a number of molecular switches.
- A collection of hematopoietic growth factors that bind to nonredundant type I transmembrane proteins from the cytokine receptor family and share structural similarity are also crucial for hematopoiesis. Some of these proteins (such as erythropoietin, granulocyte colony-stimulating factor, and thrombopoietin) are the physiological regulators of a particular lineage of blood cells, while others appear to represent redundant hematopoietic growth-promoting activities of molecules necessary for other biologic processes (e.g., interleukin-3 [IL-3], interleukin-11 [IL-11], granulocyte-macrophage colony-stimulating factor).
- At any given time, most of the HSCs are in resting stage and some enter the cell cycle. Proliferation and differentiation depend in the presence of suitable environment and other factors. WNT/β-catenin and Notch-δ signaling pathways controls the development of stem cells. Transcription factors including GATA, RUNX1, TEL/ETV6, SCL/TAL1, LMO2, PU.1, GFI1/2, C/EBPα plays important role in self renewal, differentiation, proliferation and survival of HSCs and further down the commitment cells.
- Multi-protein complex assembles together and bind the DNA regulatory elements to modulate the transcription. Epigenetic mechanisms including DNA methylation and histone methylation also has their role in controlling the process.
- Intracellular transcription factors, cell cycle regulators, and cell adhesion molecules are additional components that are all regulated by both genetic and epigenetic mechanisms.
Conditions interfering with Hematopoiesis
Hematopoiesis can be disrupted by a variety of elements and ailments, with consequences that range from minor to severe. For instance, your bone marrow may get clogged with fat deposits as you age, leaving less space for hematopoiesis.
Blood cell production can be hampered by blood conditions and blood diseases such leukemia, lymphoma, and myeloma. These could result in an abundance of unhealthy blood cells that don’t perform as they should.
Low blood cell counts can also result from medicine that interferes with hematopoiesis. Chemotherapy, for example, destroys cancer cells but also reduces your white blood cells (neutropenia). Certain drugs may cause low blood cell counts as an adverse effect.
Who is the father of hematopoiesis?
- Irving L. Weissman, MD
Weissman, MD., the first scientist to identify and isolate mammalian blood-forming stem cells in mice.
Which is the earliest site of hematopoiesis in the embryo?
- Yolk sac.
Hematopoiesis begins in the early yolk sac, but as embryogenesis progresses, the fetal liver and spleen take over this job. Later, the bone marrow takes over this function, where it continues throughout life.